Research article
Post transplant lymphoproliferative disorder: a case series and review of literature
Rizna Abdul Cader1[*], Rozita Mohd1, Halim Abdul Gafor1, Norella CT Kong1
1Nephrology Unit, Department of Internal Medicine, Universiti Kebangsaan Malaysia Medical Centre, Jalan Yaacob Latif, Bandar Tun Razak, Cheras, Kuala Lumpur 56000, MalaysiaEXCLI J 2013;12:Doc144
Abstract
Post-transplant lymphoproliferative disorder (PTLD) is a recognized complication exclusive to solid organ transplant recipients and carries a high mortality. We retrospectively reviewed records of all renal transplant recipients under follow up at our institution over the last seven years (2005-2011). We reviewed the patient characteristics, immunosuppression regimen and risk factors for the development of PTLD and its outcomes in our transplant cohort. Four out of 63 patients were diagnosed with PTLD. PTLD was incidentally diagnosed on a transplant biopsy that was performed for an unexplained rise in serum creatinine in three patients. The fourth patient presented with left submandibular lymphadenopathy. Majority presented within 18 months of renal transplantation. After the diagnosis of PTLD on graft biopsy, all patients were fully investigated and two patients had systemic involvement. In the patients with systemic involvement, reduction of immunosuppression and anti B cell therapy with Rituximab was used with good success. The patient with submandibular lymphadenopathy received chemotherapy in addition to reduction of immunosuppression. Three PTLD cases were polyclonal and diagnosed early whereas the fourth case was monoclonal. PTLD can sometimes be incidentally diagnosed on an allograft biopsy performed for rejection. The incidence of PTLD in our centre is higher than reports from other centres but our outcome is good if recognised and treated early.
Keywords: Epstein-Barr virus, immunosuppression reduction, post transplant lymphoproliferative disorder, renal transplantation
Introduction
Post-transplant lymphoproliferative disorder (PTLD) is a recognized complication exclusive to solid organ transplant recipients and is the second most common malignancy after skin cancers in these patients (Ondrus et al., 1999[15]). Malignancy is the leading cause of death after infections and cardiovascular disease in renal transplant recipients. The incidence of PTLD is about 1 % in adult renal transplant recipients but has been reported to be higher in paediatric recipients (Dharnidharka et al., 2001[6]). The incidence is lowest in renal transplant recipients compared to heart, liver or lung transplant recipients and can be as high as 6-10 % in lung transplants recipients (Mihalov et al., 1996[14]). The intensity and type of immunosuppression are associated with the development of PTLD (Dharnidharka et al., 2001[6]). Other risk factors include Epstein-Barr virus (EBV) seronegative recipients (Cockfield et al., 1993[5]; Manez et al., 1994[13]), co-existing Cytomegalovirus (CMV) infection (Manez et al.,1994[13]; Walker et al. 1995[20]), the use of monoclonal anti-CD3 antibody and cadaveric transplant recipients. Despite treatment, PTLD carries 60 % mortality (Caillard, et al., 2006[2]). Initial therapy in PTLD is immunosuppression reduction which can sometimes result in complete remission but carries the risk of rejection (Tsai et al., 2001[19]).
We noted an increase in the incidence of PTLD at our institution (Ciancio et al., 1997[4]). This prompted the review of patient characteristics, immunosuppression regimen and risk factors for the development of PTLD and its outcomes in our transplant cohort.
Patients and Methods
We retrospectively reviewed records of all renal transplant recipients under follow up at our institution over the last 7 years (2005-2011) from our database and collected data on the patients diagnosed with PTLD after renal transplantation. We collected the demographics of patients (age, gender and sex), type of renal transplant, the use and type of an induction agent, immunosuppressive regimen, renal function and age at diagnosis of PTLD. We also collected data on primary diagnosis of ESRD, time to developing PTLD, type of donor kidney, donor and recipient CMV and EBV serology, episodes of rejection, episode of calcineurin inhibitor toxicity, treatment received and outcome.
The diagnosis of PTLD was made based on histology and in most cases from a renal transplant biopsy specimen. The specimens were all reviewed by a consultant histopathologist who verified the diagnosis of PTLD.
Results
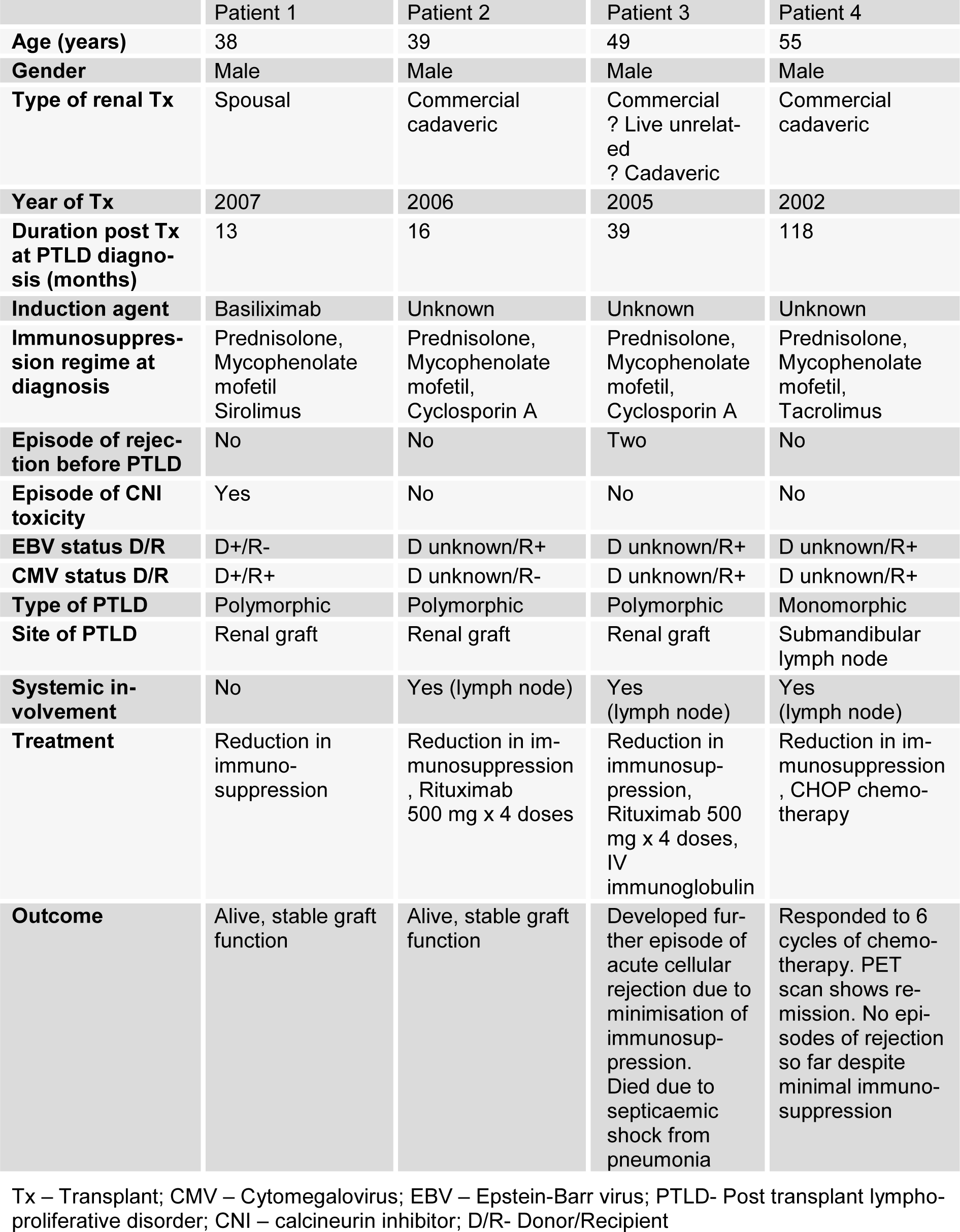
Four out of 63 patients were diagnosed with PTLD. Their demographics and characteristics are tabulated on Table 1(Tab. 1). PTLD was incidentally diagnosed on a transplant biopsy that was performed for an unexplained rise in serum creatinine in three patients. The fourth patient presented with symptoms of fever, upper respiratory tract infection and left submandibular lymphadenopathy and PTLD was diagnosed from lymph node biopsy. Once PTLD was diagnosed, patients were fully investigated and 2 patients had systemic involvement.
In most of the patients we did not have the donor details in terms of CMV and EBV serology, and type of induction agent (if used) as majority were done overseas with commercial donors.
Discussion
PTLD occurred in 6 % of our transplant patients and was notably higher in our cohort than the 1 % reported rate (Gerstenkorn et al., 2001[9]). Interestingly, the majority of our patients was asymptomatic. Three cases of PTLD were incidentally diagnosed on an allograft biopsy for an acute rise in serum creatinine. PTLD can occur within the allograft and should be considered as a differential diagnosis for acute rejection.
The incidence of PTLD varies with the organ transplanted, the presence and intensity of immunosuppression (especially Cyclosporine A based regimens), EBV seronegative recipients, co-existing CMV infection and cadaveric transplant recipients (Cockfield et al., 1993[5]; Manez et al., 1994[13]; Walker et al., 1995[20]; Izadi et al., 2011[11]; Sampaio et al., 2012[16]) The use of Muromonab-CD3 (OKT3) as an induction agent has also been associated with the development of PTLD (Cockfield et al., 1993[5]; Walker et al., 1995[20]). We believe the possible reasons for our higher incidence of PTLD are EBV infection and a higher degree of immunosuppression. Until recently, a third of all Malaysian renal transplants were commercial cadavers and therefore no data is available on the EBV status of the donor. In case 3, the patient had two previous episodes of rejection, hence the need for augmented immunosuppression. Several studies have shown a higher incidence of PTLD in paediatric renal transplant recipients as many paediatric patients are EBV naive compared to the adult population who is predominantly EBV seropositive (Dharnidharka et al., 2001[6]). Studies have demonstrated EBV seronegative pre-transplantation increases the risk of primary infection with EBV and development of PTLD increases by 76 six fold (Walker et al., 1995[21]; Sampaio et al., 2012[16]).
PTLD can be classified into a polyclonal or monoclonal proliferation of B lymphocytes or T lymphocytes (Swerdlow 1992[17]; Anonymous, 2004[1]). The majority of our PTLD cases was polyclonal and diagnosed early. PTLD starts off as polyclonal and then becomes monoclonal. Most PTLDs arise from B cell as EBV has a predilection for B cells.
The majority of our patients presented within 18 months of transplantation which is in keeping with reported data. The risk of developing PTLD is highest in the first year after solid organ transplantation when immunosuppression is at its highest and is mostly driven by EBV infection. Studies have shown that recipients with late onset PTLD frequently presented with monomorphic lesions and a significantly higher risk of disseminated disease (Izadi et al., 2011[11]). Our study found similar findings in that our first two cases presented early on with polymorphic PTLD. Patient 3 although presented late was polymorphic whereas patient 4 was monomorphic.
Allograft involvement can occur in renal transplant recipients with PTLD as evidenced by 3 of our cases with it being localized to the graft only. Khedmat and Taheri (2010[12]) demonstrated 37 % of their patients had PTLD confined to allograft and this subset of patients had better survival than other PTLD patients unless they developed multi-organ involvement. Five-year survival rate was 73 % for graft PTLD and 42 % for other localizations. Graft PTLD patients had shorter time from transplant to PTLD and were more likely to present as polyclonal and polymorphic (Khedmat and Taheri, 2010[12]). Our findings concur with this.
Treatment of PTLD involves a few regimens - the mainstay of treatment is reduction of immunosuppression in all cases although currently, there is no standardized approach (Tsai et al., 2001[19]). European guidelines recommend stopping the antimetabolite and minimizing the calcineurin inhibitor by at least 50 %, some say about 20 % every two weeks until about 30 % of the initial dose (European best practice guidelines, 2002[8]). However, immunosuppression reduction is associated with a higher risk of graft rejection and graft loss with reported rejection rates of 37 % (Tsai et al., 2001[19]). Reduction of immunosuppression allows the recovery of the recipients T cells which perform surveillance against EBV infected cells. However, response rate to immunosuppression reduction alone is low (Gerstenkorn et al., 2001[9]).
Another strategy is the treatment with antivirals in EBV driven PTLD. Estimation of EBV viral load allows pre-emptive prophylaxis by treatment with antiviral agent for at least one month and depending on viral load (European best practice guidelines, 2002[8]). However, these agents will only inhibit the lytic phase and decrease the degree of shedding of virus but the number of EBV infected cells is not altered by acyclovir treatment.
Other treatment strategies include Rituximab monotherapy in CD20-positive B-cell PTLD (Elstrom et al., 2006[7]) or CHOP-like chemotherapy (Choquet et al., 2007[3]). Hematotoxicity, leading to infectious complications and treatment-related mortality is the therapeutic limitation of CHOP. Renal graft function may be decreased at the time of diagnosis but significantly improves following treatment of the lymphoma (Trappe et al., 2009[18]). Compared with renal transplant controls with stable graft function, PTLD patients receiving chemotherapy had a non inferior graft function at follow-up (Trappe et al., 2009[18]). This suggests that the negative impact of immunosuppression reduction on graft function can be compensated by the immunosuppressive effect of CHOP, suppressing both cell-mediated and humoral immunity through its effects on T and B cells (Gholipour-Shoiili et al., 2011[10]). Conversely, patients with PTLD may be over immunosuppressed. Overall reported response rates are about 40-60 % for single agent Rituximab and up to 90 % for sequential treatment with four courses of Rituximab followed by four cycles of CHOP (Trappe et al., 2009[18]). Anti-CD20 monotherapy is therefore the preferred treatment modality in PTLD when patients fail to respond to upfront immunosuppression reduction, although they seem to be less effective in high-risk patients.
In our cohort, patients with systemic involvement received Rituximab with good response rates. In the case of patient 3 (who was also diabetic), he had been treated twice for rejection previously and therefore received higher level of immunosuppression. After the diagnosis of PTLD, we reduced his immunosuppression and treated him with Rituximab. About 18 months later, he developed another episode of cellular rejection for which he received high dose steroids, but developed recurrent septicaemia episodes and eventually succumbed to it.
Nephrectomy has been suggested for PTLD in renal allograft. Studies demonstrate that survival analysis in patients with renal allograft involvement who underwent allograft nephrectomy had a significantly better outcome compared to non nephrectomised patients (Gholipour-Shoiili et al., 2011[10]). In patients with disseminated PTLD, nephrectomy was not useful and some would consider this a drastic measure, as life on dialysis carries a significant psychosocial burden (Gholipour-Shoiili et al., 2011[10]).
Mortality has been reported to be over 50 % (Caillard et al., 2006[2]). Meta-analysis in liver transplant recipients have reported one and five years survival rate for early onset PTLD to be 64 % and 54 % respectively (Izadi and Taheri, 2011[11]).
Conclusion
PTLD can sometimes be incidentally diagnosed on an allograft biopsy that was performed for rejection. Therefore renal transplant recipients who develop allograft dysfunction during the early post-transplantation period should be investigated for potential PTLD development at their allograft site. The outcome is good if recognized and treated early.
References
[*] Corresponding Author:
Dr. Rizna Abdul Cader, Nephrology Unit, Department of Internal Medicine, Universiti Kebangsaan Malaysia Medical Centre, Jalan Yaacob Latif, Bandar Tun Razak, Cheras, Kuala Lumpur 56000, Malaysia, eMail: Rizna_c@hotmail.com