Research article
Factors affecting the adoption of healthcare information technology
Nisakorn Phichitchaisopa1, Thanakorn Naenna2[*]
1Technology of Information System Management, Faculty of Engineering, Mahidol University, Nakhonpathom 73170, Thailand2Department of Industrial Engineering, Faculty of Engineering, Mahidol University, Nakhonpathom 73170, Thailand
EXCLI J 2013;12:Doc413
Abstract
In order to improve the quality and performance of healthcare services, healthcare information technology is among the most important technology in healthcare supply chain management. This study sets out to apply and test the Unified Theory of Acceptance and Use of Technology (UTAUT), to examine the factors influencing healthcare Information Technology (IT) services. A structured questionnaire was developed and distributed to healthcare representatives in each province surveyed in Thailand. Data collected from 400 employees including physicians, nurses, and hospital staff members were tested the model using structural equation modeling technique. The results found that the factors with a significant effect are performance expectancy, effort expectancy and facilitating conditions. They were also found to have a significant impact on behavioral intention to use the acceptance healthcare technology. In addition, in Thai provincial areas, positive significance was found with two factors: social influence on behavioral intention and facilitating conditions to direct using behavior. Based on research findings, in order for healthcare information technology to be widely adopted and used by healthcare staffs in healthcare supply chain management, the healthcare organizational management should improve healthcare staffs' behavioral intention and facilitating conditions.
Keywords: Healthcare Information Technology, technology acceptance, Unified Theory of Acceptance and Use of Technology (UTAUT)
Introduction
Healthcare technology is among the most important equipment in a hospital. It helps to improve the quality and performance of treatments (Calman et al., 2007[9]). Furthermore, it affects indirect profit added to hospitals. For instance, electronic medical records (EMR) and computerized provider order entries (CPOE) can decrease the time necessary or care processing steps, especially when retrieving information (Holden, 2010[27]). Some previous research studies have discovered that if healthcare services do not adopt new information technology for additional support, they will be ineffective, and lose credibility among patients (Aggelidis and Chatzoglou, 2009[2]; Lu et al., 2005[35]; Ammenwerth et al., 2003[5]). Therefore, information technology needs to be applied to healthcare services.
It can also be useful in health center activities. Physicians can operate these technologies to access diagnostic data or to prescribe medicine for transactions via healthcare systems. Healthcare technologies can decrease medical errors, identify patients, manage physician/nurse teams, and improve service quality and safety (Holden, 2010[27]; Chen et al., 2007[11]; Fisher and Monahan, 2008[23]). Thus, healthcare technologies are needed in the healthcare services to provide quality services.
Healthcare systems and healthcare quality must support patients who want treatment that provides high quality and safety. Healthcare quality affects the level of satisfaction regarding acceptable behavioral choices for ordinary patients. Satisfaction and service in healthcare quality depend on the quality of the management system (Naidu, 2009[ref:40]). In research conducted in Turkey, it was found that patients in private hospitals express greater satisfaction with the service of physicians, nurses and support services with up-to-date medical technology. Private hospital services are preferred over government hospital services (Taner and Antony, 2006[48]). Technology increases data connections between hospitals, physician officers, health centers, pharmacies and patients. It also improves usage for patients who travel and/or move, which will improve therapeutic methods (McDonald et al., 2005[37]). Thus, healthcare management and medical technology services will be improved. Physicians, nurses and medical technicians should also have technological skills to gain maximum benefit.
The technology acceptance model has been widely adopted within information technology and applied to many industries. Over the past decade, researchers have defined factors for technology acceptance and various behaviors in using information technologies. The factor results, which were found to be affected within the research, have been adopted in other industries such as healthcare (Kijsanayotin et al., 2009[31]; Janz and Hennington, 2007[28]; Wu et al., 2007[57]), banking (Zhou et al., 2010[60]; AbuShanab and Pearson, 2007[1]) and government services (Lean et al., 2009[32]). We found results from tests with the technology acceptance model, such as the Technology Acceptance Model (TAM), the theory of planned behavior (TPB) and the Unified Theory of Acceptance and Use of Technology (UTAUT) (Venkatesh et al., 2003[55]). Other researchers have tested technology acceptance in healthcare organizations (Chang et al., 2007[10]; Pai and Huang, 2011[44]; Wu et al., 2007[57]). They studied these technology acceptance factors in order to improve the standards of service and quality in healthcare.
Prior research studies have suggested that technology acceptance is suitable for finding the factors influencing acceptance. The technology acceptance model is suitable for using modeling tools including predictions, attitudes, satisfaction, and usage based on beliefs and external variables (Al-Gahtani and King, 1999[4]). Additionally, we should specifically study the factors influencing healthcare technology.
The theoretical background is divided as follows: the first section presents healthcare technology, the second section explains technology acceptance, the third section presents the Unified Theory of Acceptance and Use of Technology (UTAUT), and the last section explains provincial areas and technology acceptance in this research.
Materials and Methods
Healthcare technology
Nowadays, healthcare technology has become the highest growing area in the healthcare industry, and in offering employment opportunities in healthcare. Spetz and Maiuro (2004[47]) define healthcare technology equipment in healthcare according to dependent variables by theories with no dimensions. So, healthcare technology should be up-to-date. It helps to attract more patients. Therefore, healthcare can also adopt technology in order to utilize competitive strategies with other healthcare systems. Within the context of healthcare technology, Van Bemmel (Van Bemmel and Musen, 1997[53]; Hanson, 2006[25]) offers to divide healthcare technology according to each healthcare process. It is divided as follows:
First, both communication and telemetrics comprise level 1, which is defined as a technology or system that can help in telecommunications both inside and outside of hospitals. The results from lab tests can be immediately sent to a nursing station or nursing ward. So, that a physician can evaluate the condition of a patient, and can initiate immediate medical services. The speed of communication depends on the speed of information technology in the organization. The technology at this level is related to data acquisition, transmission coding, decoding processes and encoding processes. For example, most healthcare services use a Local Area Network (LAN) to transfer laboratory test results, including lab testing from clinicians' tests and transfers from physicians' prescriptions to the pharmacy department.
Next, storage and retrieval of databases comprise level 2, this technology level can be defined as data recording. Most hospitals use Electronic Health Records (EHR), which form a real-time system for recording data, such as medical imaging records, patients' history files, and past medical prescriptions. The EHR helps physicians and nurses by providing access to patients' health record information, so that they can make decisions easier and faster by incorporating evidence-based support for those decisions (Davis, 2007[ref:16]). There are four main databases: patient databases, hospital databases, nationwide databases, and knowledge databases.
Subsequently, processing and automation comprise level 3, these technologies or tools are related to processing diagnoses or therapies such as x-ray therapy, blood banks, and mammography. In medical service laboratories, microprocessors inside of medical laboratory devices can self-analyze and transfer results to the central laboratory computer, which then produces role control quantities and reports. The laboratory automation also includes a blood and urine sample bar code reading device. It also scopes the processing of biological signals. It includes computer processing to tackle mathematical and physical problems and quality control. Example of computer processing data and automation include nuclear medicine tests and Positron Emission Tomography (PET scan).
After that, diagnosis and decision-making linked to therapy which comprise level 4. They are technologies used to analyze and construct the best treatment for each patient decision. Examples of this information technology include computed tomography (CT scanner) and ultrasound.
Next, therapy and control comprise level 5, this technology is used for patient therapies such as cardiac cauterization, lithotripsy, and angioplasty, etc. This level includes automatic control of fluid balance in a post-operative intensive care unit (ICU). Some research teams work on implantable microsystems. For instance, Self-energizing Implantable Medical Microsystems (SIMM); this tool is operated by balloon. It is installed in the heart chamber. This technology level also includes: ICU close look fluid monitoring, insulin pumps, demand pacemakers, and implanted special purpose computers, etc.
Finally, level 6 is comprised of related research and modeling. This level is used for operational research, and using the results to treat patients with transplantation issues from laboratories that transplant human issue (Vazquezsalceda et al., 2003[54]), such as the blast cyst center.
The information technology in this study is considerably related with two levels of healthcare technology: level 1 and level 2. Level 1 focuses on communication technology for healthcare staff such as connecting internally and externally. Level 2 focuses on storage databases for storing healthcare data on patients, treatment process, and medicines.
Technology acceptance
Many theories are concerned with information technology acceptance such as the Theory of Reasoned Action (TRA), Technology Acceptance Model (TAM), Theory of Planned Behavior (TPB), Extended Technology Acceptance Model (TAM2), and the last technology acceptance model is “The Unified Theory of Acceptance and Use of Technology (UTAUT)”.
One of the most fundamental and influential theories on human behavior is the TRA. This theory includes two core constructs: i) Attitude toward behavior and ii) Subjective norms. Attitude toward behavior is defined as “an individual's positive or negative feeling (evaluate affect) about performing the target behavior”. Subjective norm is defined as “the person's perception that most people who are important to him/her think he/her should or should not perform the behavior in question” (Fishbein and Ajzen, 1975[22]).
The TPB, TAM and UTAUT use the TRA construct that Behavioral Intention (BI) is used for predicting users' behavior of what technologies they will use. BI is the main determinant for measuring the degree of intention in using those technologies or in making a decision. It is considered based on the individual behavior of the user and other related factors.
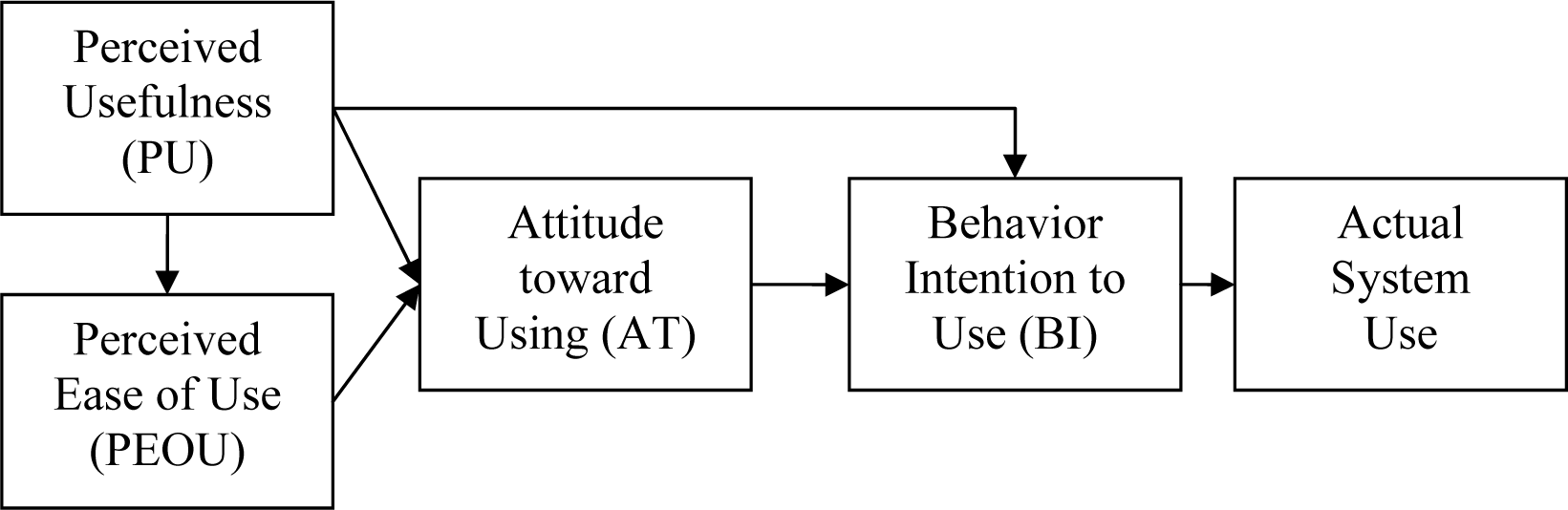
Davis (1989[17]) developed the Technology Acceptance Model (TAM) (see Figure 1(Fig. 1)). This theory is based on the TRA (Fishbein and Ajzen, 1975[22]). The TAM includes two determinants: i) perceived usefulness (PU) and ii) perceived ease of use (PEOU). These are related to the behavior of individuals, and can be forecasted by BI, which is the determinant of reliability and acceptance in information technology (IT) or in decision-making. The TAM provides a basis for tracing the external impact that variables have on internal beliefs, attitudes, and intentions (Davis et al., 1989[18]).
Next, Venkatesh et al. (2003[55]) tested the hypotheses of the eight theories for finding beneficial factors. They developed an IT acceptance theory. It is called “The Unified Theory of Acceptance and Use of Technology (UTAUT)”.
The Theory of Planned Behavior (TPB) extended the TRA by adding the construct of perceived Behavioral Control (Ajzen, 1991[3]). Attitude toward behavior and subjective norm are adopted from the TRA. Perceived Behavioral Control is defined as the perceived ease of performing the behavior. In addition, individual behavior is considered BI on Attitude, Subjective norm and perceived Behavioral Control. Ajzen presented a review of several studies that successfully used the TPB to predict intention and behavior in a wide variety of settings. The TPB has been successfully applied to the understanding of individual acceptance and usage of many different technologies (Harrison et al., 1997[26]; Mathieson, 1991[36]; Taylor and Todd, 1995[50]).
Human behavior theories vary widely, Triandis (1977[52]) presented a perspective to add to those proposed by the TRA and TPB. Thomson et al. (1991[51]) adopted and refined Trandis' model for IS contexts, and used the model to predict PC utilization. The Model of PC Utilization (MICU) is suitable for predicting individual acceptance and use of different levels of information technology.
Moore and Benbasat (1991[39]) adapted the characteristics of the Innovation Diffusion Theory (IDT) in 1991. This theory initially defines the individual based on attitudes towards a specific (e.g. technological) innovation, which in turn, leads to the decision whether to choose to adopt. This theory explains from an individual perspective, a person's attitude towards the innovation technology, whether each person will decide to adopt these technological advances. Therefore, it is frequently studied alongside technological innovations.
Davis et al. developed the Motivation Model (MM) in 1992. The Motivation Model is a significant body of research in psychology supported by general motivation theory as an explanation for behavior (Davis et al., 1992[16]). Next, the Combined TAM and TPB (C-TAM-TPB) combine the predictors from TPB with perceived usefulness from TAM to provide a hybrid model (Taylor and Todd, 1995[49]).
Social Cognitive Theory (SCT) was developed in 1997 by Bandura and Adams. They found five main factors: Outcome Expectations-Performance, Outcome Expectations-Personal, Self-efficacy, Affect and Anxiety (Bandura and Adams, 1997[6]). First, Outcome Expectation-Performance is defined as the performance that people expect for efficiency in job-related outcomes. Second, Outcome Expectation-Personal is defined as the effect of performance on behavior. Especially, individual expectations dealing with self-esteem and achievement signals. Third, Self-efficacy is the determination to develop the ability to use a form of technology, e.g., computers, mp3 players, etc. Fourth, Affect is an individual's favorite particular behavior to engage in, e.g., listening to a favorite song on an iPod. And last, Anxiety is defined as evoking anxious or emotional reactions when performing a behavior, e.g., stress when approaching unfamiliar technology . The theory has been tested in regard to other learning technologies (Compeau et al., 1995[15][14], 1999[13]).
Next we will compare the four determinants of UTAUT and acceptance theories affect on behavioral intention (BI). First, Performance Expectancy uses the same determinants as perceived usefulness (from TAM, TAM2, and C-TAM-TPB), Job fit (from MPCU), Relative advantage (from IDT), Extrinsic Motivation (from MM), and Outcome expectation (from SCT). Second, Effort Expectancy also uses the same determinants, such as Perceived ease of use (from TAM, TAM2), Complexity (from MPCU), and Ease of use (from IDT). Third, Social Influence is similar to Subjective norm (from TAM2, TRA, TPB/DPTB, and C-TAM-TPB), Social factors (MPCU), and Image (from IDT). And finally, the Facilitating Conditions determinant is also the same as Perceived Behavioral Control (from TPB/DPTB, and C-TAM-TPB), and Compatibility (from IDT). We can conclude the determinants by comparing these with other technology acceptance models as in Table 1(Tab. 1)(Venkatesh et al., 2003[55]).
UTAUT
The Unified Theory of Acceptance and Use of Technology (UTAUT) was developed from eight theories, which include the Theory of Reasoned Action (TRA), Technology Acceptance Model (TAM), Motivational Model (MM), Theory of Planned Behavior (TPB), Combined TAM-TPB (C-TAM-TPB), Model of PC Utilization (MPCU), Innovation Diffusion Theory (IDT) and Social Cognitive Theory (SCT) (Venkatesh et al., 2003[55]). They introduced it as a new IT acceptance theory.
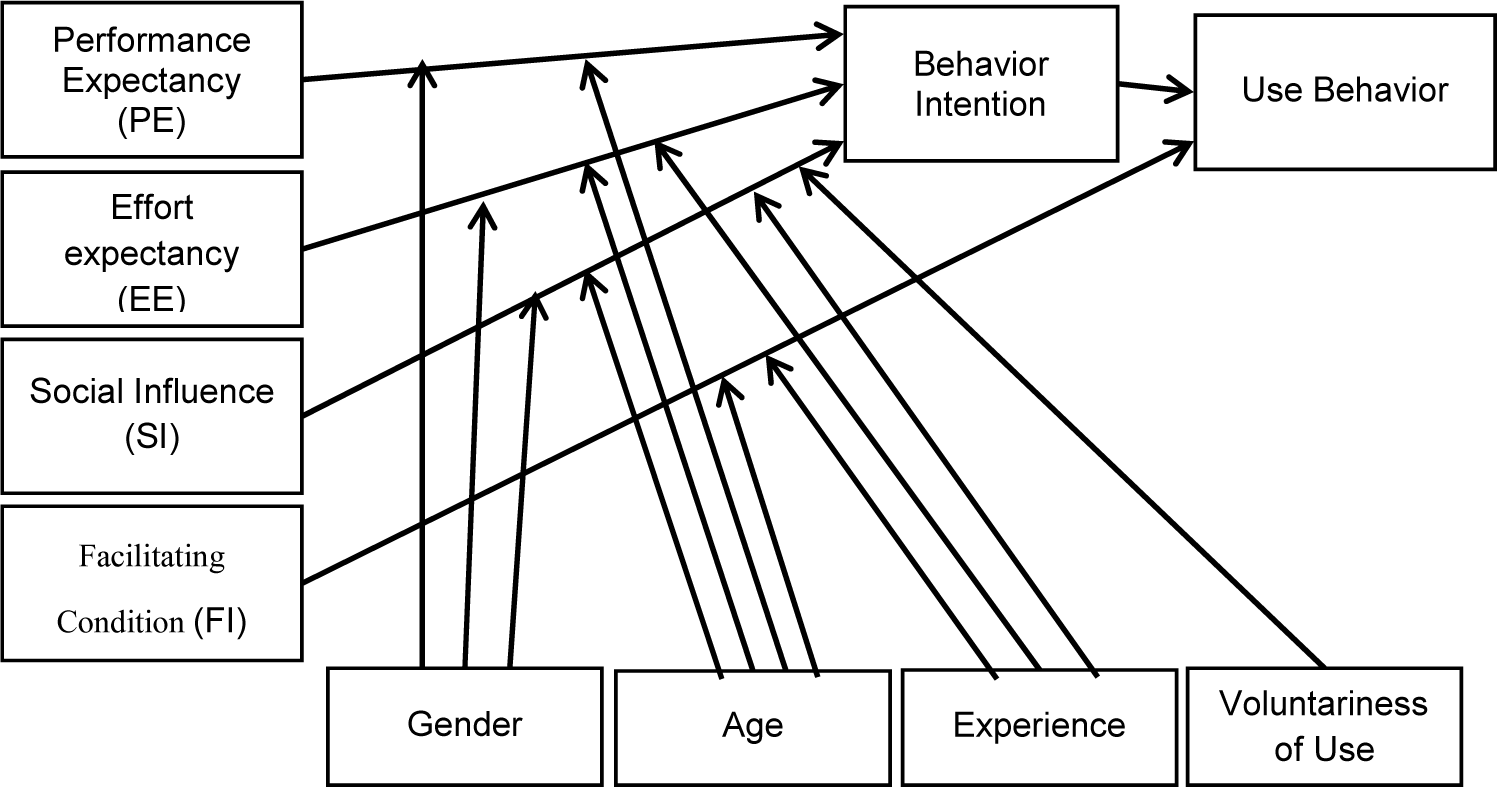
Figure 2(Fig. 2) illustrates that the UTAUT proposes four main determinants of behavioral intention regarding people using information technology, which are Performance Expectancy (PE), Effort Expectancy (EE), Social Influence (SI), and Facilitating Conditions (FI). In addition, the UTAUT model found four moderators which affect the determinants: gender, age, experience and voluntariness of use from the perspective of social psychology.
Performance Expectancy is defined as the performance of information technology for the user. Effort expectancy is defined as the degree of ease associated with use of the system. Social influence is defined as the degree to which an individual perceives the importance that others give to whether he or she should use the new system. Social influence is considered to be system or application-specific, whereas subjective norm relates to non-system-specific factors. Facilitation Conditions are defined as the degree to which an individual believes that an organization and/or technical infrastructure exist to support their use of the system (Venkatesh et al., 2003[55]).
External variable: Provincial areas and technology acceptance
The provincial areas in a country make a difference in the overall level of technology acceptance. For example, healthcare in the capital can be found to have up-to-date technology and support from healthcare administrators. It can also support ease of use of the technology. Different access to technology in the provincial areas of a country has an effect on behavioral intention. Based on previous research, it was found that India and the United States have different technological cultures, including provincial areas, and it was found that the culture of the provincial areas affect behavioral intention to use technology (Kakoli and Soumava, 2008[30]). When cultural identity invokes different characteristics for each provincial area and country, there will be a contrast in how people access technology. For instance, Chinese and British students are affected by using the internet and computers, including their ability to access knowledge and their level of perceived usefulness. The difference between cultures in students has been studied distinctly for the purpose of technology (Li and Kirkup, 2007[34]). Additionally, cross-cultural differences have a considerable effect on technology acceptance factors. For example, some research indicates that social influence has a significant impact on all country samples. It shows that cross-cultural differences affect actual results (Oshlyansky et al., 2007[43]). Therefore, cross-cultural differences are suitable for research on technology acceptance. It will be useful for countries with many provincial areas, such as China or Thailand. In addition, Thailand has different cultures present in each provincial area. Provincial areas have differences in various fields such as access to technology, local dialects, and local foods. Hence, we also are interested in studying culture, as it is a modulator of technology acceptance factors.
Research Model and Hypotheses
Research model
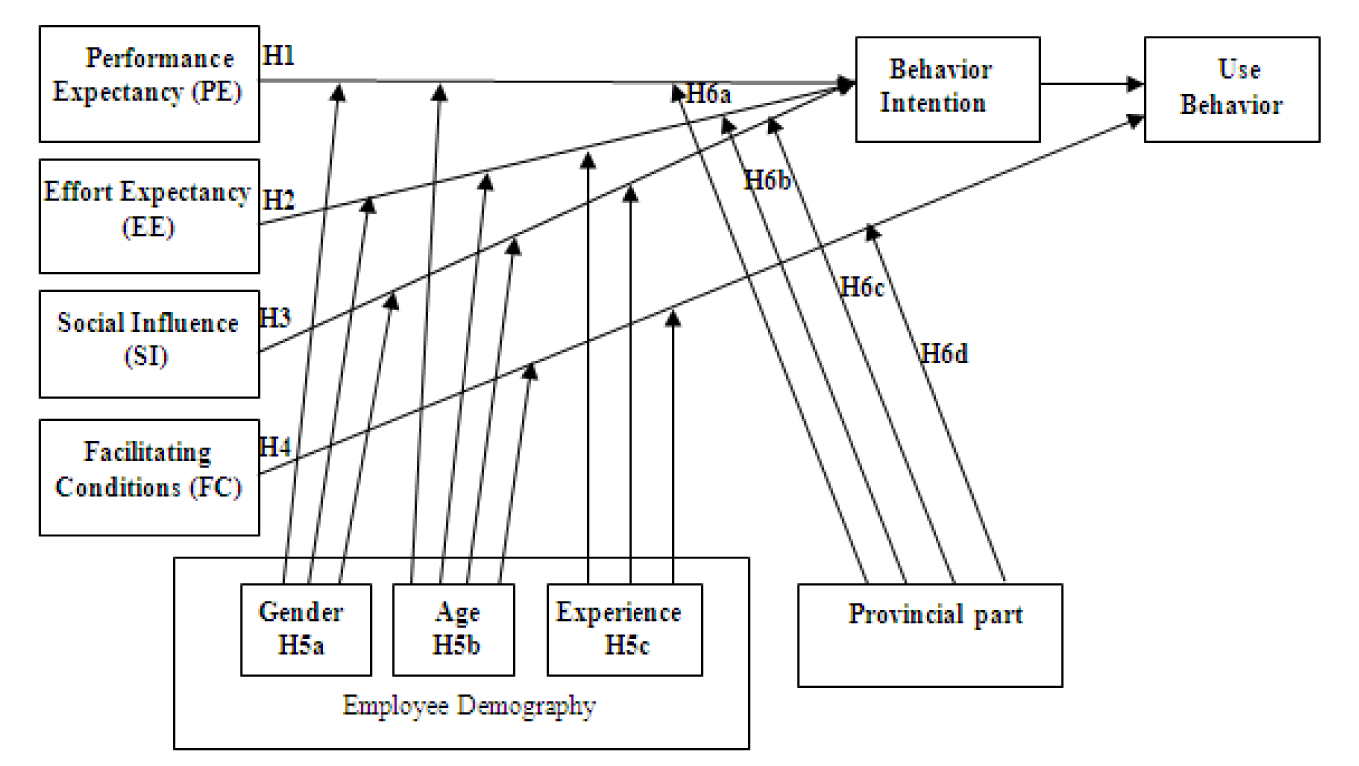
In this study, Figure 3(Fig. 3) presents the research model and hypotheses, which were expanded based on the Unified Theory of Acceptance and Use of Technology. The main UTAUT factors include performance expectancy, effort expectancy, social influence, and facilitating conditions. External factors also are explained by provincial areas and employee demographics.
Performance Expectancy refers to the performance of information technology and associated systems for users. In Taiwan, research has been conducted about physicians 'acceptance of pharmacokinetics-based clinical decision support systems'. Chang et al. (2007[10]) found that in Taiwan, performance expectancy affected behavioral intention to use more strongly than expectancy. Yi et al. (2006[58]) have found that perceived usefulness affects Behavioral Intention with use of PDAs by physicians in the United States. Pai and Huang (2011[44]) also found that perceived usefulness had a positive direct effect on intention to use. Therefore, it follows that:
H1: Performance Expectancy positively affects Behavioral Intention to use healthcare technology.
Effort expectancy is considered to be directly associated with ease use of the system. Many early research studies found that effort expectancy affects the usage of systems. It was found that effort expectancy has a positive significant effect on intention to use clinical decision support systems (Chang et al., 2007[10]), healthcare information systems (Pai and Huang, 2011[44]), and adverse event reporting systems (Wu et al., 2008[56]). Thus, it follows that:
H2: Effort Expectancy is positively related to Behavioral Intention to use healthcare technology.
Social Influence refers to beliefs as to whether an individual should use a system. It has been found in other technology acceptance models, such as the TRA, TPB and DTPB. From research on acceptance of hospital information systems (HIS) (Aggelidis and Chatzoglou, 2009[2]), it was found that social influence affects the behavioral intention of hospital personnel. Wu et al. (2008[56]) also indicated that subjective norm had a direct positive effect on Behavioral Intention in using an adverse event reporting system. Accordingly, a hypothesis is presented as follows:
H3: Social Influence positively affects Behavioral Intention to use healthcare technology.
Facilitating Conditions are circumstances that an individual believes exist to support his/her activities, such as the infrastructure or environment. Chang et al. (2007[10]) showed that Facilitating Conditions have a positive effect on physicians' use behavior of pharmacokinetics-based clinical decision support systems. Yi et al. (2006[58]) found that Perceived Behavioral Control (PBC) was a significant determinant of Behavioral Intention to use PDAs in physicians. Facilitating Conditions were represented by the PBC as a direct determinant of use. Therefore, we hypothesized:
H4: Facilitating Conditions positively influence “Use Behavior”.
Employee demographics are defined as the characteristics of healthcare staff. With the UTAUT hypothesis, we have four main factors which define relationships with other moderators. The moderators consisted of age, gender, voluntariness and experience. These moderators have been shown to affect intention to adopt by other research studies (Kijsanayotin et al., 2009[31]; Venkatesh et al., 2003[55]; Yu et al., 2009[59]; Burtonjones and Hubona, 2006[8]). We dropped voluntariness from the UTAUT moderators and are only using the three moderators. Based on past research results, a hypothesis is presented as follows:
H5a: Age positively influences (PE, EE and SI) and Behavioral Intention to use healthcare technology.
H5b: Gender positively influences (PE, EE, and SI) and Behavioral Intention to use healthcare technology. And, Gender positively influences Facilitating Conditions on “Use Behavior”.
H5c: Experience positively influences (EE, SI and FC) and on Behavioral Intention to use healthcare technology. And, Experience positively influences Facilitating Conditions on “Use Behavior”.
There are many research studies that are related to provincial areas and technology acceptance. Kakoli and Soumava (2008[30]) studied user acceptance of prepayment between India and United States. These two countries are very different. They found that performance expectancy, effort expectancy, and social influence positively affect users' intention to use the prepayment system. Each of these countries, along with the different cultures within the countries, were found to have effects on behavioral intention. Oshlyansky et al. (2007[43]) studied technology acceptance cross-culturally. There were nine countries sampled cross-culturally: the Czech Republic, Greece, India, Malaysia, New Zealand, Saudi Arabia, South Africa, United Kingdom, and the United States. They found that social influence affects website acceptance in Saudi Arabia more than in the other countries. Consequently, there are four hypotheses which were developed according to the research model as follows:
H6a: Provincial areas are positively influenced by Performance Expectancy in Behavioral Intention to use healthcare technology.
H6b: Provincial areas are positively influenced by Effort Expectancy in Behavioral Intention to use healthcare technology.
H6c: Provincial areas are positively influenced by Social influence in Behavioral Intention to use healthcare technology.
H6d: Provincial areas are positively influenced by Facilitating Conditions in “Use Behavior”.
Research Methods
Instrument designs
Researchers inspected the following six determinants of healthcare technology acceptance: performance expectancy, effort expectancy, social influence, facilitating conditions, behavioral intention and healthcare technology behavior usage; and, modulators were also included, such as age and gender. In our study, healthcare technology acceptance is defined as each physician and healthcare staff members' use of healthcare technology in healthcare.
The questionnaireAppendix A.pdf was divided into three parts: demographic respondent profiles, healthcare profiles, and affected factor items. First, the demographic questions ask for age, gender, education, position, employment experience, and internet experience. Next, healthcare profile inquires about data regarding hospital type and the location of healthcare e.g., Bangkok. And last, the affected factor items were scale items for examining the determinants.
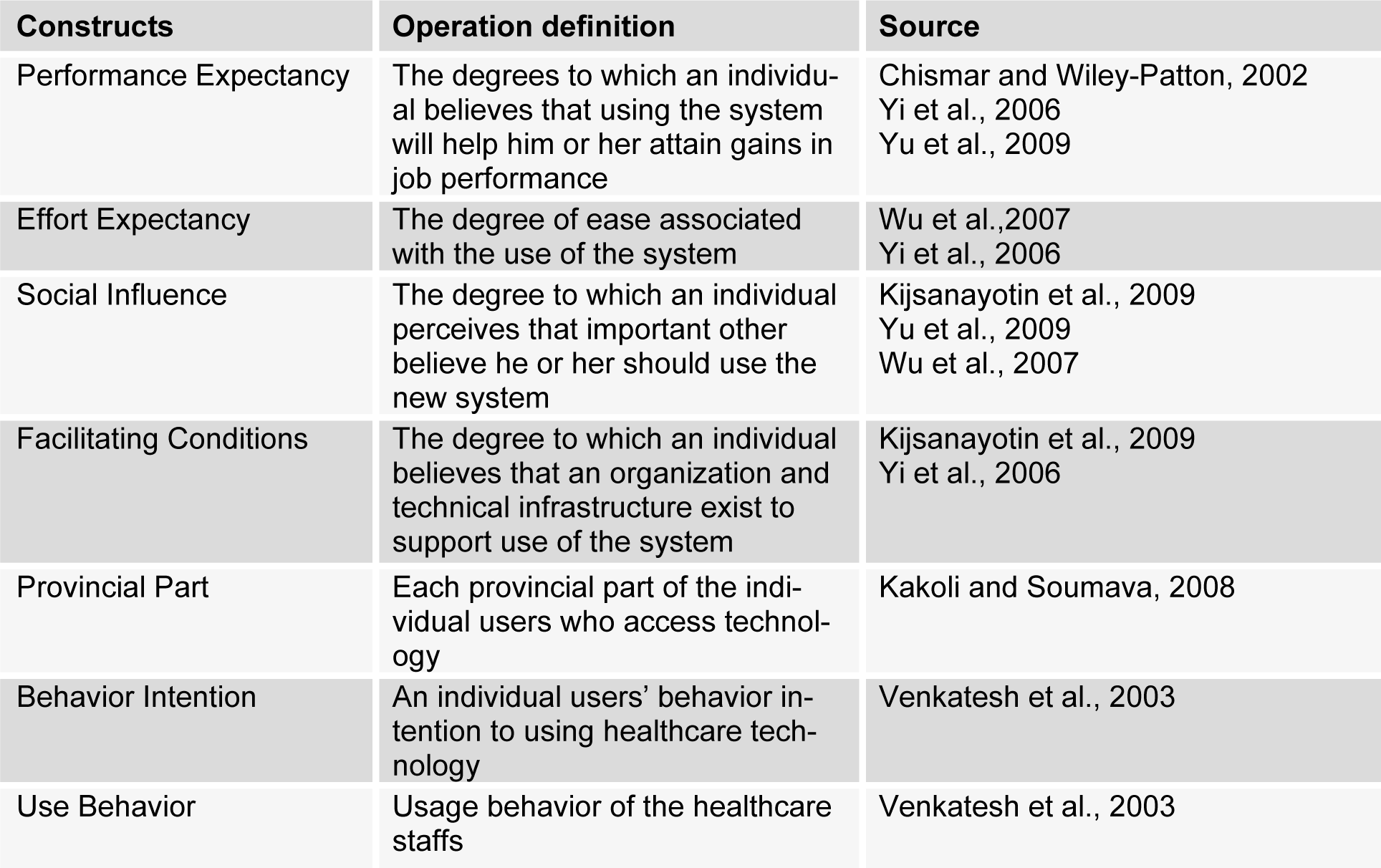
Table 2(Tab. 2) shows the operation definitions of construct items. Each item was measured. A five-point Likert type scale was adopted with anchors ranging from “strongly disagree” (1) to “strongly agree” (5).
Subject and sampling
The subjects for this study included users of information technology in healthcare technology, including physicians, nurses, and healthcare staff members who work for hospitals in each provincial area of Thailand. The randomly sampled population weighed provincial areas of Thailand: Bangkok, middle, north, northeast and south. The questionnaires were sent to targets to gather data by letters, interviews, and online questionnaires. Of the 800 questionnaires which we sent out, 437 questionnaires were returned. Incomplete questionnaires were removed. The 400 completed questionnaires yielded a total response rate comprising 50 % of the primary sample.
Data analysis method
The monitored data for use in the analysis is important to the research. It helps to identify errors in the data among the examined hypotheses. After all of the data has been collected, tests must be conducted in order to check reliability and validity.
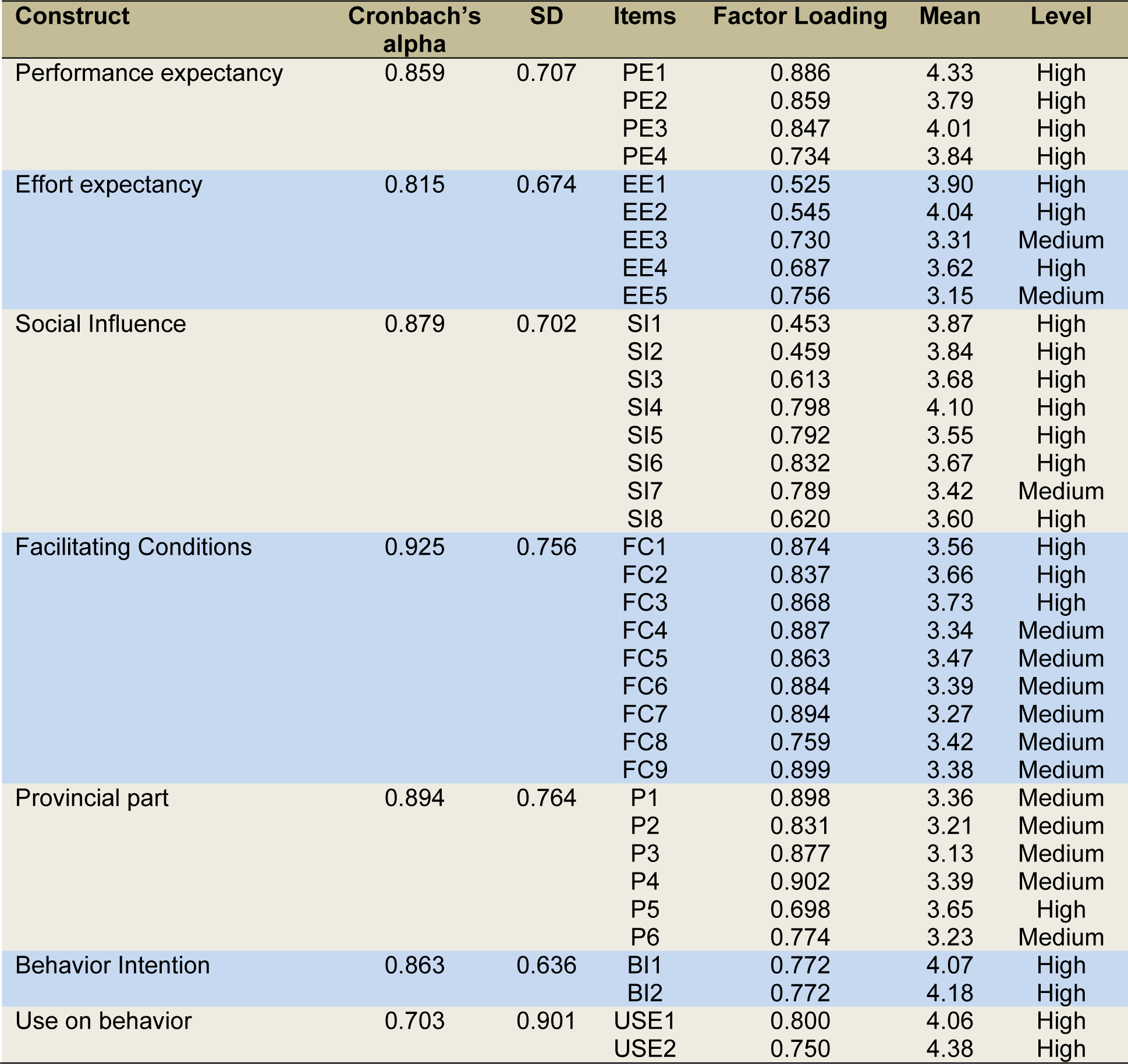
Factor loading, composite reliability and variance extracted measures examined the convergent validity of the measurement items. Factor loading of all items in each construct range must exceed the recommended value of 0.70. Therefore, the measurement items can be shown to have convergent validity.
The reliability analysis obtained using Cronbach's alpha value was above the value of 0.70 (Nunnally, 1978[42]), as shown in Table 3(Tab. 3). This shows that the questionnaire has good reliability and validity of the measurement model.
Reliability was tested using the composite reliability results. As shown in Table 3(Tab. 3), almost of the values were above 0.70. This indicates the confirmed acceptable level in this research. Nevertheless, Falk and Miller (1992[21]) also suggested that reliability factor loading values should have a value level of 0.55. In Table 3(Tab. 3), the majority of value constructs were approximately or over 0.70, with the exception of the three constructs of Social Influence which were 0.453 and 0.459, which is less than 0.50. Finally, the results proved the composite validity of the measurement model with respect to the model's constructs.
SPSS 16.0 was used for descriptive statistics of the variables (Norusis, 2008[41]), Lisrel 8.8 was used to examine their factors in the hypotheses.
Results
Characteristics of the respondents
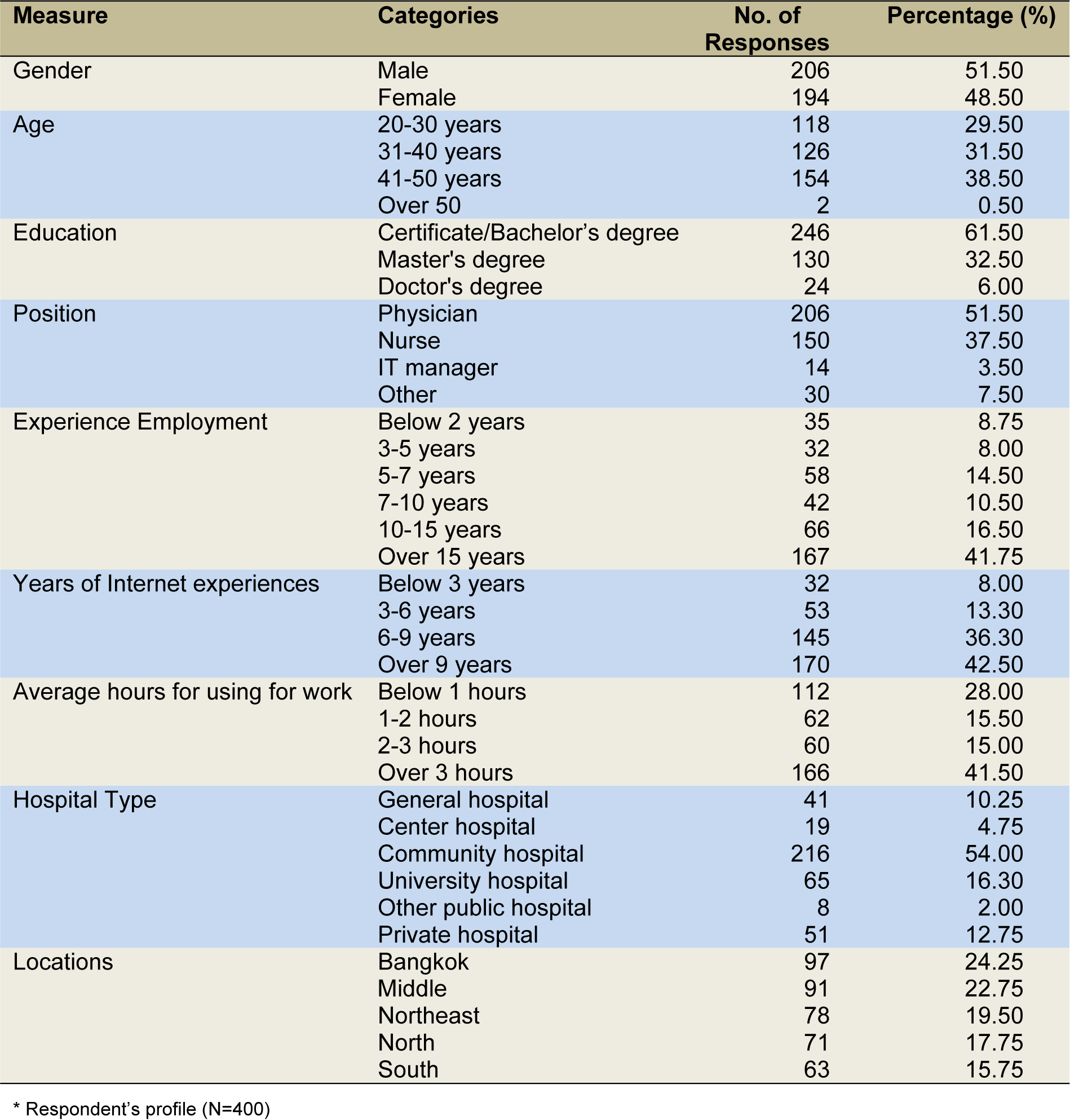
Data were gathered from physicians and healthcare staff members who work in healthcare in each provincial area in Thailand. The profiles of the respondents are shown in Table 4(Tab. 4), with a total sample size of 400. The data indicate that the respondents consisted of males (51.5 %) and females (48.5 %). Based on the respondent information, the majority were between 41-50 years old (38.50 %), followed by those between 31-40 years old (31.5 %), closely followed by those between 21-30 years old (29.5 %) and a small minority who were over 50 (0.5 %). With regard to education levels, it was found that the majority of respondents had a certificate or bachelor's degree (61.5 %), and that more than half were physicians (51.5 %). For routine activities among healthcare staff members, it was found that most work for over 3 hours (41.5 %).
For most of the respondents, those who use healthcare technology had an internet and healthcare technology experience.
Preliminary structural equation model
A Structural Equation Model (SEM) was found to be suitable to test and confirm the results of the theoretical hypothesis (Jöreskog and Sörbom, 1996[29]). Structural equation modeling, or Confirmatory factor analysis (CFA), were used to test the sufficiency of the measurement model by Lisrel 8.8 (student version). The sufficiency of the measurement model was examined according to the model fit and the relationship among the variables.
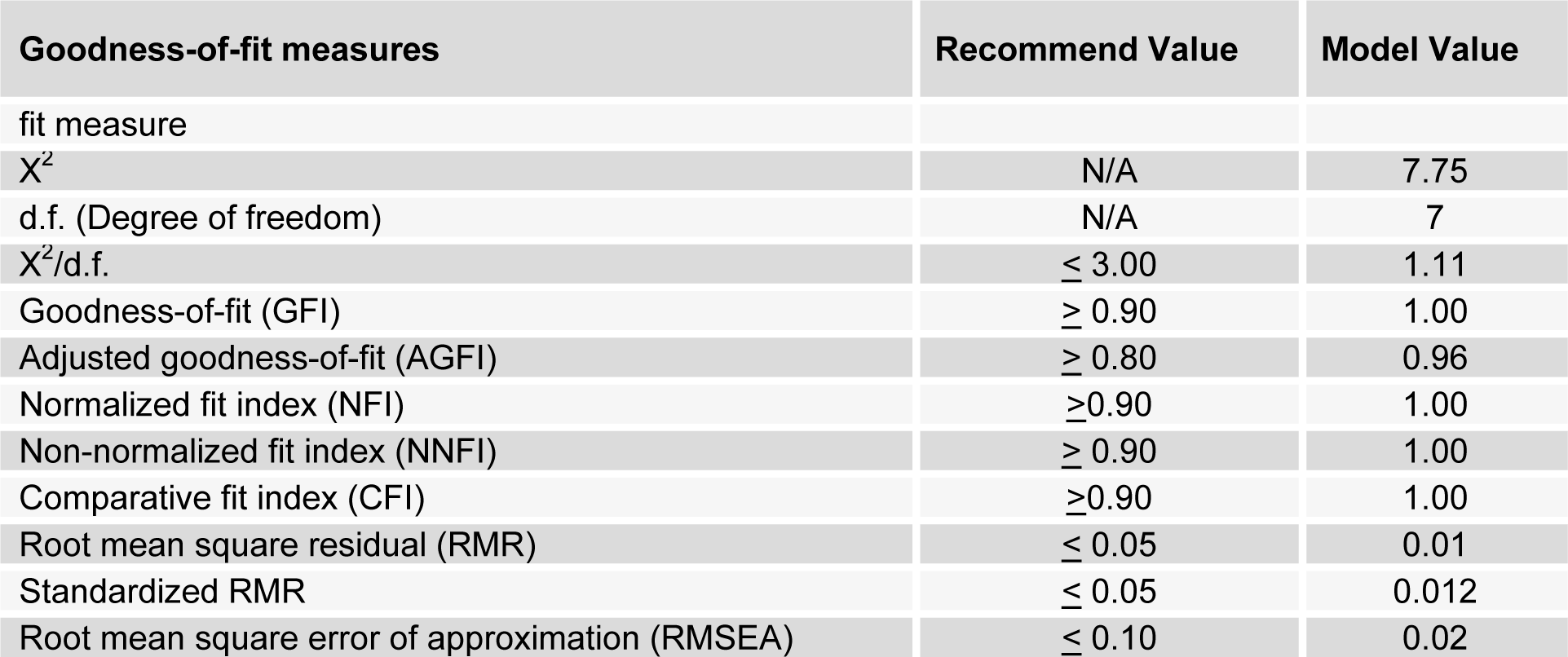
For a good model fit, the Chi-square value was normalized by a degree of freedom (Χ2/d.f.) value of 1.11. Goodness-of-fit was 1.00. Adjusted goodness-of-fit (AGFI) was 0.96. Normalized fit index (NFI) was 1.00. Non-normalized fit index (NNFI) was 1.00. Comparative fit index (CFI) was 1.00. Root mean square residual (RMR) was 0.01. Standardized RMR was 0.012, and Root mean square error of approximation (RMSEA) was 0.02 (see Table 5(Tab. 5)).
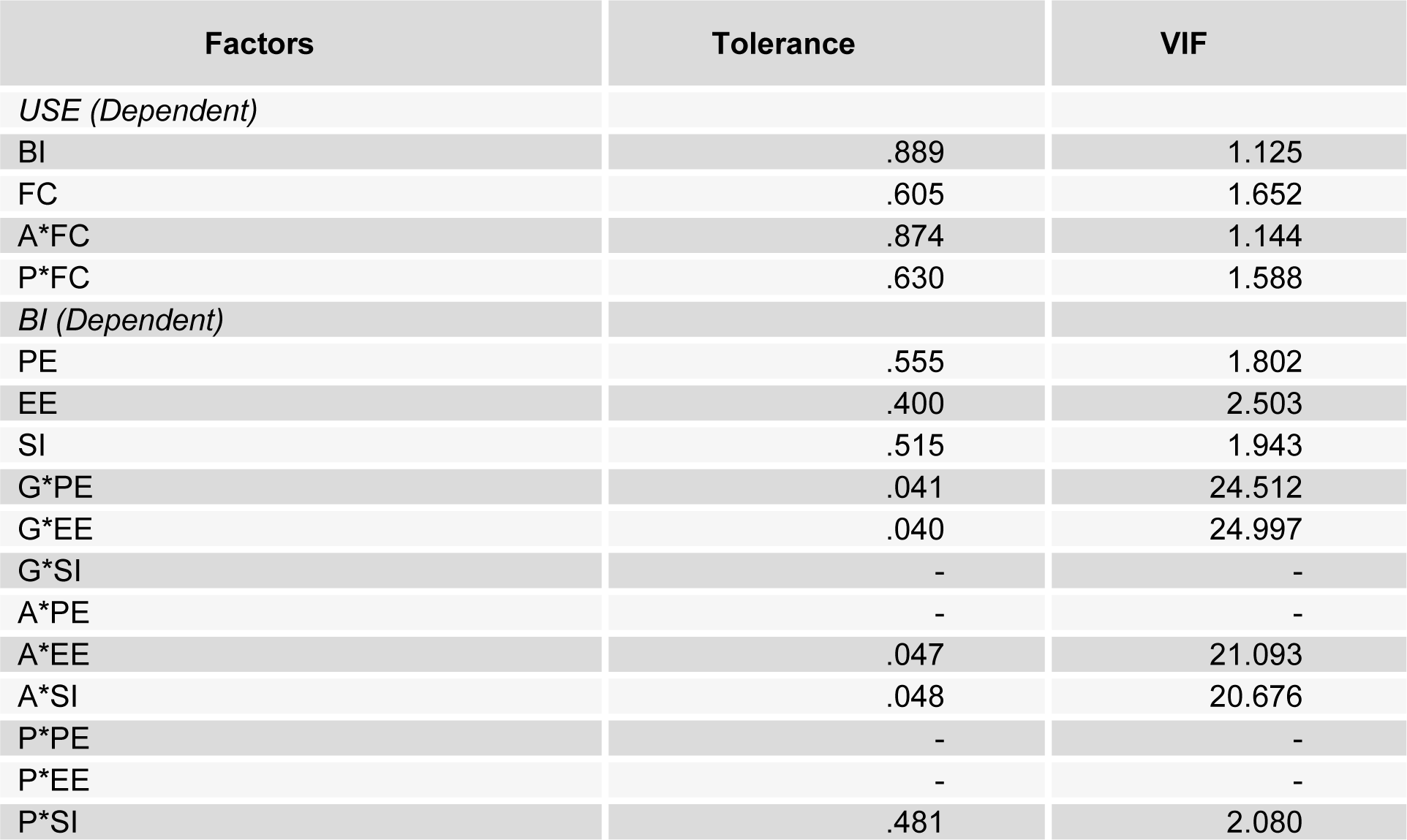
A preliminary test found the Tolerance and Variance Inflation Factor (VIF) for checking multicollinearity. When the tolerance value is close to zero, there is high multicollinearity of that variable with other variables, and the beta co-efficient will be unstable (Hair et al., 1998[24]). Conversely, the VIF is higher than the inter-correlation of the variables.
This indicates that there was almost no multicollinearity problem with these variables. Although some values were not standard, they were dummy variables. These results follow in Table 6(Tab. 6).
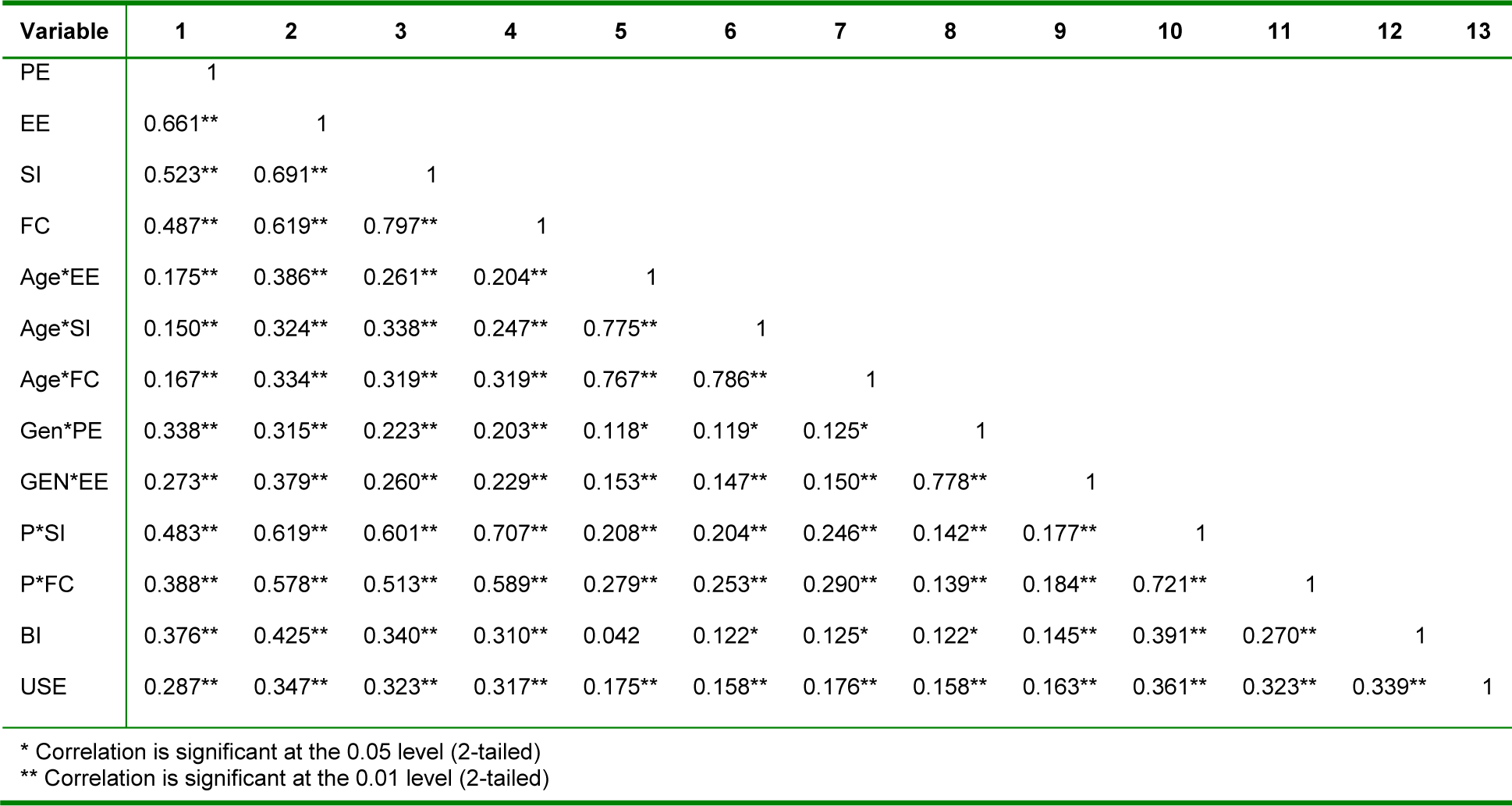
To check the relationships between the variables, the data was analyzed by employing correlations. This analysis found that all independent variables had poor relationships with each other, and that there were highly accurate relationships between the independent and dependent variables. Consequently, the variables were suitable for analysis as shown in Table 7(Tab. 7).
Hypothesis testing
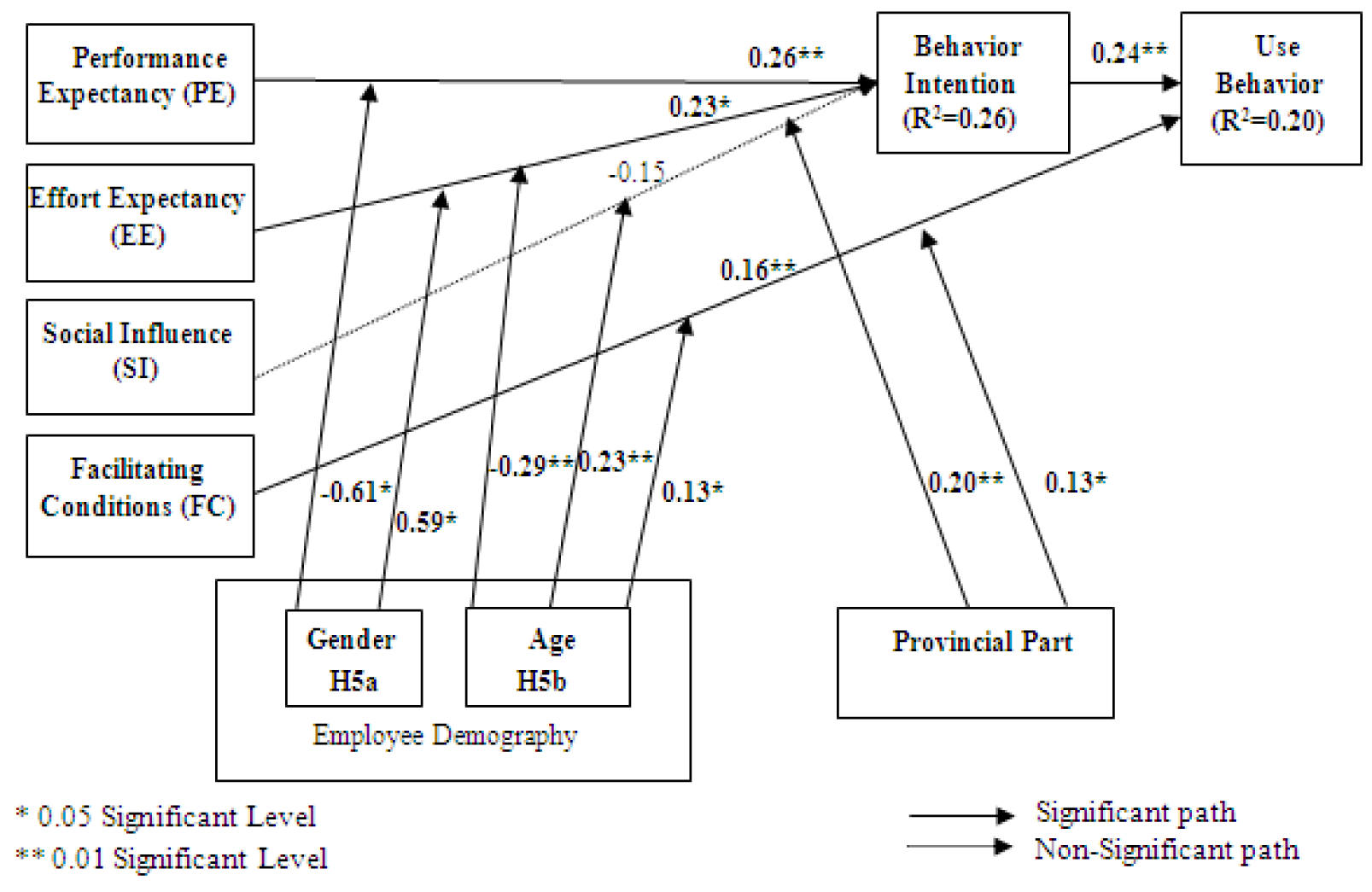
Structural equation modeling was applied to examine the hypothesis model using Lisrel. The final model (Figure 4(Fig. 4)) shows the results of the affected factors with the non-significant paths removed.
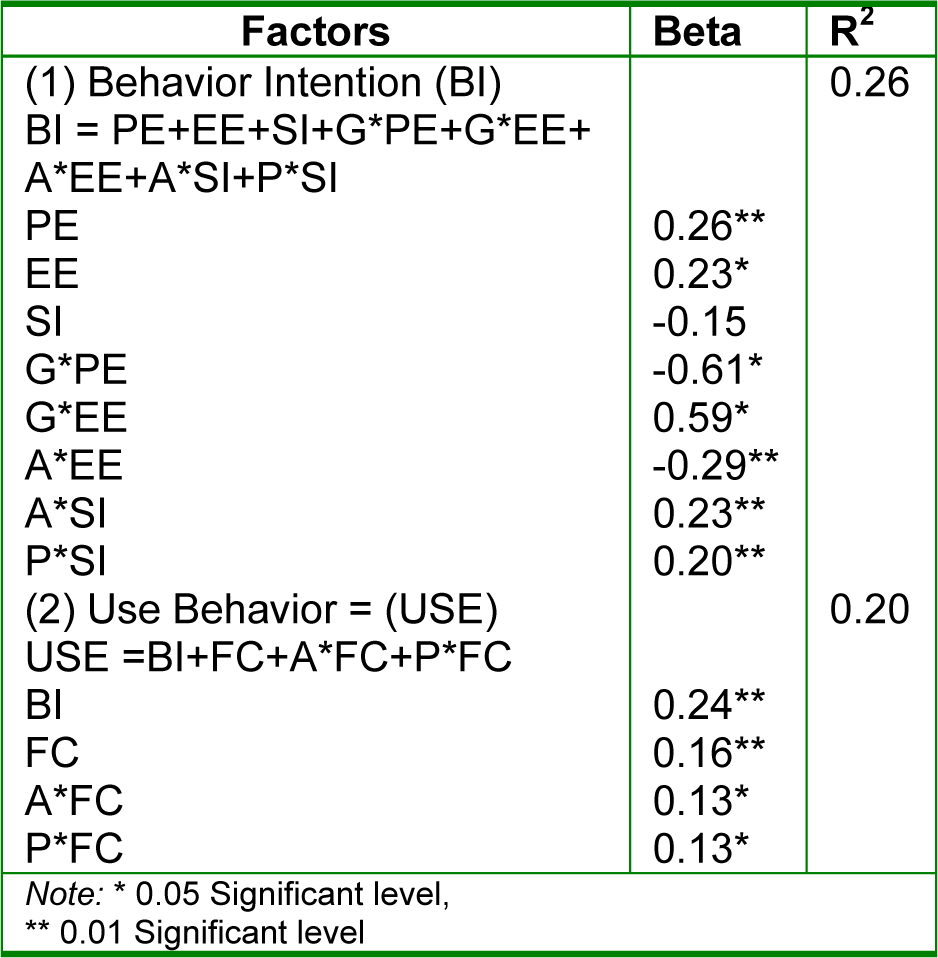
Figure 4(Fig. 4) presents the structural model results with construct variables and modulators (e.g. age, gender and provincial area) included. Using the results of the total explained variance (R2) we examined behavioral intention and using behavior, which are 26 % and 20 %, respectively. These results indicate that the structural model is satisfactory, in that it confirmed the suggestion of Falk and Miller for level of variance explained (R2> 0.1 and predictor variable explaining ≥ 1.5 % of variance) (Falk and Miller, 1992[21]). The majority of the hypotheses were strongly supported, except for hypotheses H3, H5a3 and H5c. The results indicate that the technology acceptance of users with regards to performance expectancy (H1; β = 0.26, p < 0.01), and effort expectancy (H2; β = 0.23, p < 0.05), respectively, positively affected behavioral intention towards actual usage behavior of healthcare staff in accepting healthcare technology. In addition, the facilitating conditions (H4; β = 0.16, p < 0.01) were also found to positively affect actual usage behavior among healthcare staff members. However, social influence which is a minimum construct, had an insignificant (H3; β = -0.15) influence on behavioral intention.
For the modulators, we found that provincial areas are indirectly affected by social influence (H6c; β = 0.20, p < 0.01) and facilitating conditions (H6d; β = 0.13, p < 0.05). These constructs also have an influence on behavioral intention and using behavior. The employee demographics consisted of gender and age, respectively. If the gender was found to be negatively significant, then it is representative of female gender. Female gender was also found to affect performance expectancy. Next, male gender was found to affect effort expectancy in behavioral intention of people's healthcare usage behavior. If age was found to be negatively significant, it was representative of those over 40 years. Thus, an age over 40 affects effort expectancy with regard to behavioral intention. Additionally, an age of less than 40 affects social influence with regard to behavioral intention among facilitating conditions of using behaviors.
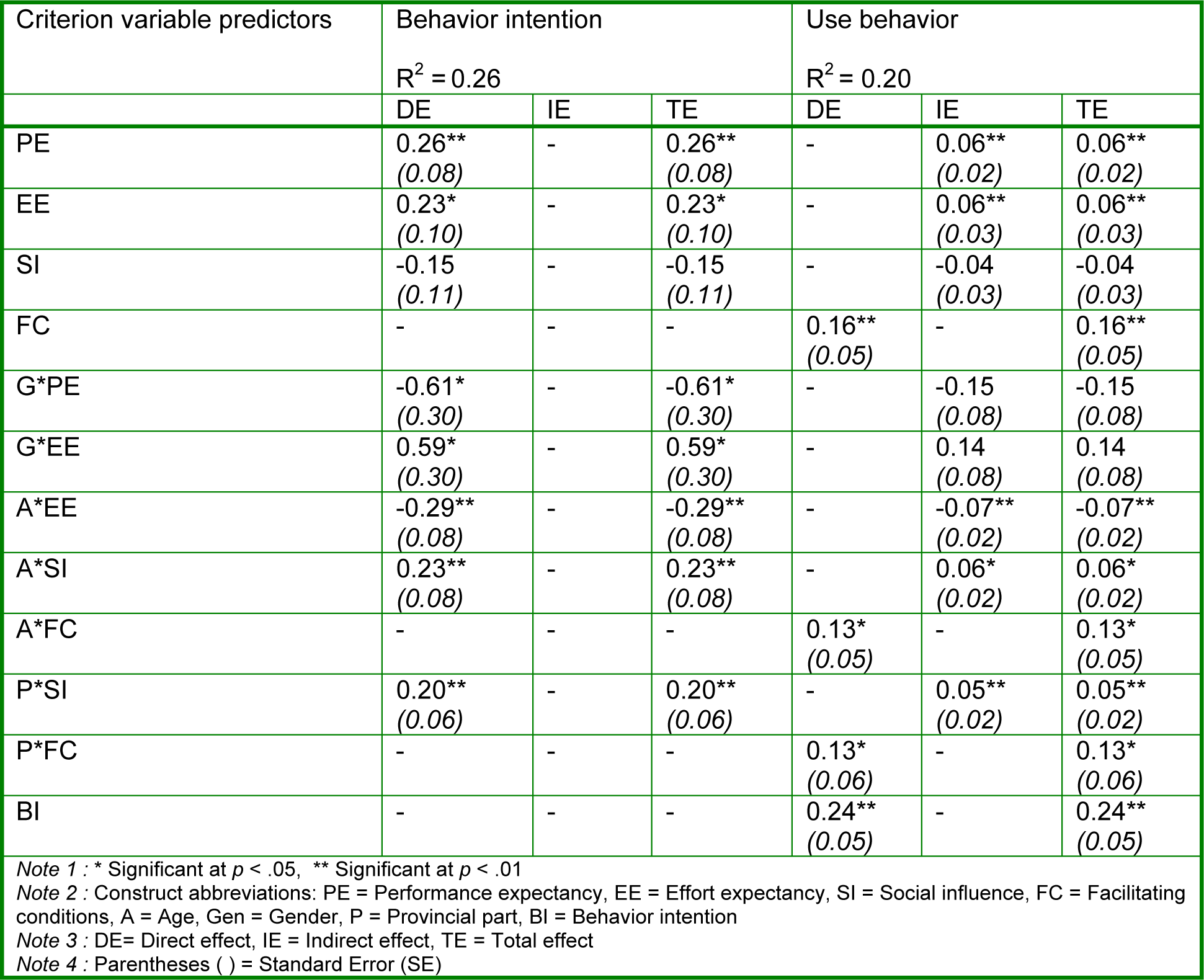
In conclusion, of the 20 hypotheses tested in the initial model, 7 were deleted from the model, while 11 of the hypotheses were found to be significant. Finally, these research results also support other previous research studies. All results are shown in Table 8(Tab. 8).
Of the majority of constructs, performance expectancy had the strongest direct effect on behavioral intention, followed by effort expectancy. This indicates that healthcare technology can support medical staff in hospitals and healthcare services, until they realize the value of using technology. Use behavior received the most direct effect from behavioral intention and facilitating conditions, respectively. Social influence may have an insignificant effect on the behavioral intention of users. But, it also has little effect on the behavioral intention of medical staff members (see Table 9(Tab. 9)).
Discussion
This study offered the UTAUT theory to explore the determinants which influence adoption of healthcare technology. The results indicate that the main factors are performance expectancy, effort expectancy, and facilitating conditions which act as significant determinants to users' behavioral intention. Moreover, the modulators included were gender, age, and provincial area, which also indirectly affected the majority factors. Performance expectancy was found to have the strongest direct effect on behavioral intention, whereas social influence was found to have no direct effect on behavioral intention, as well as no directly significant effect on total use of healthcare technology behavior. However, age and provincial areas, are modulators which have an indirect effect on social influence of users' behavioral intent. As well, age also affects effort expectancy and facilitating conditions. In addition, gender also has an indirect effect on both performance expectancy and effort expectancy; meanwhile, provincial area directly affects facilitating conditions.
The results showed that performance expectancy had the strongest effect on behavioral intention of all the main determinants. The results are consistent with previous studies (Venkatesh et al., 2003[55]; Chang et al., 2007[10]; Yi et al., 2006[58]). Healthcare technology helps support services, including medical care in the healthcare industry. Physicians use robotic surgery methods when caring for patients in such fields as gynecology and oncology. Robot surgery is one part of healthcare technology. It will limit both the time and space required for these procedures, and make complicated processes become easier (Schreuder and Verheijen, 2009[46]). Physicians will be able to treat patients correctly and quickly. Patients will have less bleeding, and secure, safe and small wounds. Thus, patients also get well more quickly and are able to return to their lives ordinarily and happily. It increases satisfaction between physicians and patients. Therefore, they believe that using healthcare technology will enhance the performance of healthcare services (Venkatesh et al., 2003[55]; Davis, 1989[19]). Similar findings were also made by Chang et al. (2007[10]). Their study indicated that physicians' trust in their prescriptions will be truly accepted. Healthcare staff members will adopt healthcare technology for services which they perceive will be useful, based on actual usage. Therefore, when users believe that using healthcare technology will increase efficiency, they will make use of it to provide good service for patients.
Healthcare staff received a high degree of usefulness from healthcare technology. These results suggest that healthcare technology influences actual usage of services within hospitals. Thus, healthcare staff should be motivated to make use of healthcare technology since it improves performance by decreasing errors and time necessary for treatment. Accordingly, choice of healthcare technology and training should be a point of focus. From the beginning of its use, healthcare staff members should participate in the choice of technology. Once chosen, healthcare technology becomes implemented within the hospital process. Training is also needed to explain the usefulness of these healthcare technologies to healthcare so that they benefit more highly.
The impact of effort expectancy on behavioral intention was found to be a factor with less of an effect than performance expectancy. This result is in accordance with prior findings (Chang et al., 2007[10]; Davis, 1989[19]; Moore and Benbasat, 1991[39]; Lee and Chao, 2004[33]). A key aspect of healthcare technology is its ease of use. Both physicians and nurses use computerized physician order entry (CPOE); this application provides the ability to write orders online. It increases legibility, and can be used to identify patient descriptions, such as aliments or medicines. Pharmacists will be able to read physicians' orders easily and immediately. It also reduces medical errors and the frequency of adverse drug effects (Bates, 2000[7]). Physicians gain support through CPOE for an easier, faster, and more accurate process for making decisions carefully. Therefore, information and service quality are also related to perceived ease of use (DeLone and McLean, 2003[20]). It also affected usage and physician satisfaction, according to their feelings about whether it is easier to use conventional methods. And finally, they also perceive ease of use in performing their job.
The results of the research demonstrate that healthcare staff members should have perceived ease of use regarding healthcare technology. Firstly, healthcare technology should be easy to use, by simplifying tasks for learning and mastering the system, making it easier to remember how to perform system tasks, and improving flexibility of use. Secondly, the function of healthcare technologies should be uncomplicated and flexible according to usage. Systems for responding and searching systems are not difficult to use. Information and data can also be managed in a clear and systematic way by healthcare staff. And finally, healthcare staff members must also acquire serious training regarding perceived understanding as technology increases. After healthcare staff members have been trained to use the healthcare technology, they will be able to perceive its ease to use by themselves. They will feel convenient with actual usage, and their acceptance will also increase.
Different social influences were found to have no significant effects on behavioral intentions, which do not show direct similarities to the findings on healthcare technology acceptance research. The result is consistent with a previous study conducted by Chismar and Wiley-Patton (2002[12]) about internet adoption. In their study, social norms and image are similar to the social influence determinants in the UTAUT. Healthcare staff members do not need to perceive pressure from social influences. Their decision to adopt healthcare technology is not influenced by pressure from other people in healthcare. Chang et al. (2007[10]) also presented findings that social influence has less of an effect on behavioral intention for technology acceptance in target physicians. The majority of target physicians showed high egos and proficient technical skills. Physicians demonstrated expert technical skills, which affected the research. In addition, the limited time available to physicians and nurses also affects interactions and minimizes exchanges. Furthermore, medical experts do not need to gain benefit from using these healthcare technologies, because they also perceived their usefulness and ease of use.
The impact of facilitating conditions has a positive influence on actual using behavior. This is in line with the results of previous studies (Kijsanayotin et al., 2009[31]; Zhou et al., 2010[60]; Rouibah et al., 2009[45]). This implies that infrastructure support, such as computer systems or knowledge are necessary. Internal and external organizations encourage physicians to allow healthcare technology to affect their behavior. Health information technology policy includes important aspects which support adoption by healthcare staff (Menachemi et al., 2011[38]). The internal organizations involved in healthcare support provide technical assistance for using healthcare technology through IT staff. IT staff in healthcare work as technology support assistants for physicians. Some physicians may have part of the knowledge necessary to operate healthcare technology, but not enough. Therefore, IT staff should also be employed in healthcare in order to provide support for healthcare technology. External organizations, such as the Ministry of Public Health, can help to improve IT in terms of healthcare, prices, and providers. They can support software centralization provided by the Ministry of Public Health for healthcare technology that has been chosen to be suitable in the country for training purposes. Finally, healthcare staff members accept healthcare technology into hospitals. Thus, it helps reducing barriers to usenew information technology for healthcare services (Chang et al., 2007[10]). Additionally, IT utilization facilitates physical behavioral intentions (Taylor and Todd, 1995[49]). Therefore, healthcare staff should receive support from internal and external organizations, such as IT staff and technical resources. Thus, the majority of participants accept all support given and feel satisfaction for it.
For the results, the modulators are demographics and provincial areas. For performance expectancy, the research results differ from the UTAUT findings with respect to the moderator of gender. Almost all of the female members of the hospital staff in Thailand are nurses. Mainly, nurses play a participatory role in helping physicians emphasize treatments. Nurses must be more attentive to the use of technology in their work than physicians. Consequently, females who are part of the healthcare staff should focus on explaining the benefits of healthcare technology rather than the processes involved.
Besides, the male group and those older than 40 were affected by these modulators with regards to effort expectancy. This suggests that they should demonstrate an understanding of healthcare technology usage, as well as its convenience, ease of use and lack of uncomplications; until they would like for it to be usable. Almost all those surveyed who were male and in the older age group were physicians. Physicians mainly have the important role of treating patients. The researcher expects that physicians' time is limited, therefore they want their work with technology to be easy. Sometimes, physicians want to be able to find information by themselves. Therefore, there are many reasons that provide motivation for studying healthcare technology.
Although social influence factors were not found to directly affect behavioral intention, the modulators of younger age and provincial area did have an effect. The main reason for this being is that the new generation of hospital staff works with colleagues of similar ages who always use new technology. In addition, in each provincial area, new physicians are often the leaders in bringing new healthcare technology to the hospital. Thus, healthcare should be of interest to new physicians.
New findings of modulators in this research reveal that provincial areas have a positive influence of facilitating conditions in the using behavior of healthcare staff members. As found by Kakoli and Soumava (2008[30]) in their study of prepayment acceptance in two countries, there were contrasts in access of technology use between the countries. Countries or provincial areas build different ways to access technology. While as our research demonstrates with the UTAUT, the findings only showed social influence and facilitating conditions. Healthcare staff members are influenced by participants in each provincial area until they are led to actual using behavior. Therefore, healthcare participants, such as hospital administrations in provincial areas also have an important role with healthcare staff members. Besides, facilitating conditions should support each provincial area to be equal in areas such as hardware, software, and IT staff. For example, hospital administrators may define policy regarding IT staff, such as salary or benefits.
Conclusions
The quality and performance of technology helps hospital employees to perceive its usefulness. Therefore, technology in healthcare should provide support with good quality, through service and information technology that perform data processing well. They should feel the perceived usefulness of healthcare technology. Some healthcare systems do not have a large enough budget for these technologies. They can choose support through performance expectancy factors. Healthcare participants must also support and provide equal services for actual healthcare users to develop excellent technical skills and a sufficient basis in healthcare technology. Eventually, healthcare in Thailand will reach the goal of operating at an international level.
Acknowledgements
This research was supported by the Office of the Higher Education Commission and Mahidol University under the National Research Universities Initiative.
References
File-Attachments
- Appendix A.pdf (44,73 KB)
Appendix A
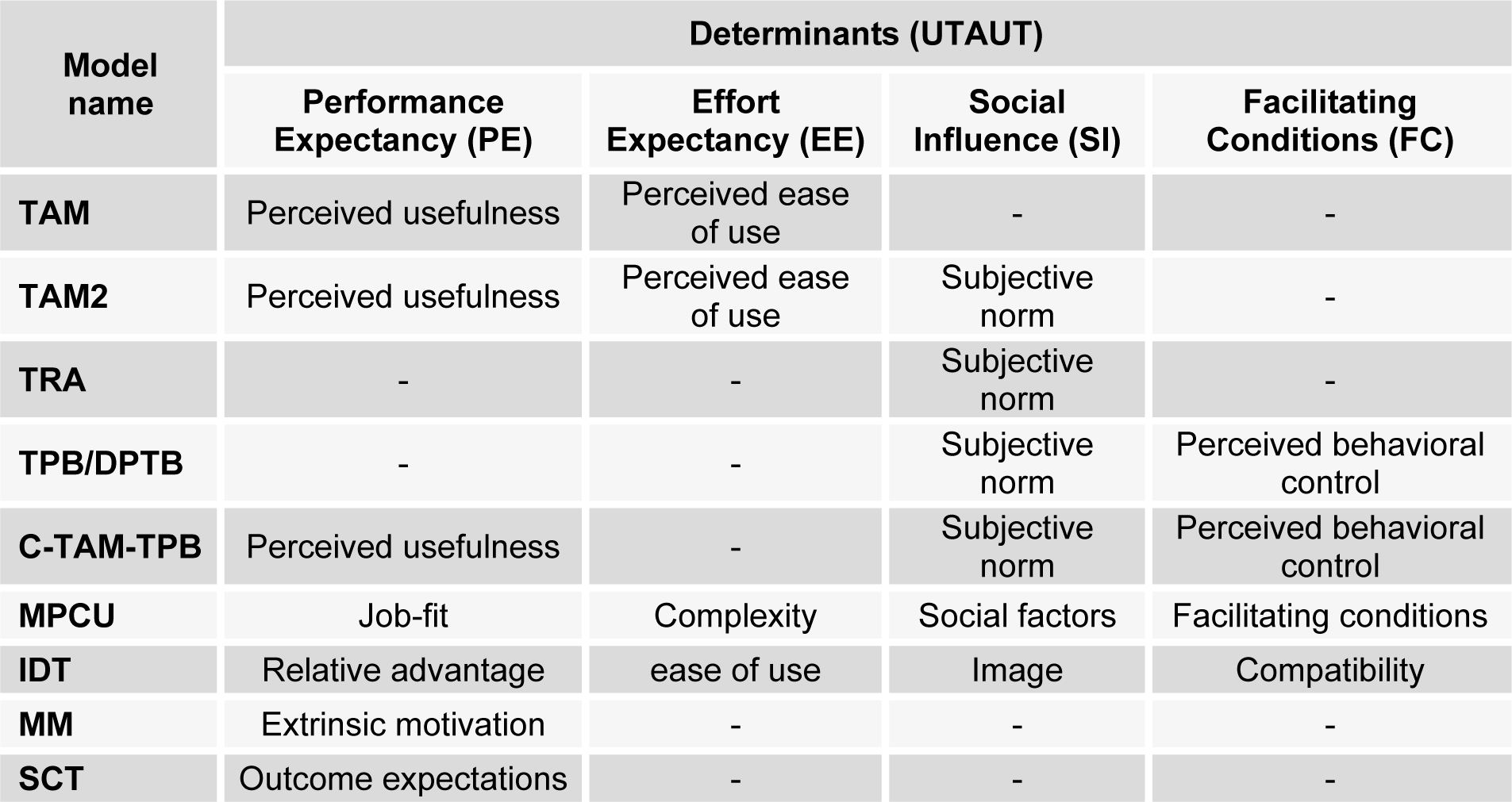
Table 1: Comparing the determinants of UTAUT with other technology acceptance models (Venkatesh et al., 2003)
[*] Corresponding Author:
Thanakorn Naenna, Department of Industrial Engineering, Faculty of Engineering, Mahidol University, Nakhonpathom 73170, Thailand; Tel: +662-889-2138 Ext 6211; fax: +662-8892-138 Ext. 6229, eMail: thanakorn.nae@mahidol.ac.th