Case report
Familial pattern of large vestibular aqueduct syndrome in a Chinese family
Mohd Hazmi1[*], A. Ab Aziz2, A. Asma1
1Department of Otorhinolaryngology, Universiti Kebangsaan Malaysia, Jalan Yaacob Latif, 56000 Cheras, Kuala Lumpur, Malaysia2Department of Radiology, Universiti Kebangsaan Malaysia, Jalan Yaacob Latif, 56000 Cheras, Kuala Lumpur, Malaysia
EXCLI J 2013;12:Doc118
Abstract
Large Vestibular Aqueduct Syndrome (LVAS) is the most common radiographic malformation in children with early onset of hearing loss. Usually its occurrence is non-familial, however intriguingly a portion of patients with LVAS is found to have evidence of genetic predisposition. We described cases of LVAS in two siblings of a Chinese family. The elder sister first presented with reduced hearing since childhood and her brother has a similar complaint upon further questioning. Their hearing test showed bilateral sensorineural hearing loss (SNHL) and computed tomography (CT) of temporal bone showed enlarged vestibular aqueduct in both patients. We described an approach to diagnosis of LVAS and highlight the importance of hearing assessment in genetic link hearing loss.
Keywords: Large Vestibular Aqueduct Syndrome, sensorineural hearing loss, computed tomography
Introduction
Large vestibular aqueduct syndrome (LVAS) or enlarged vestibular aqueduct syndrome (EVAS) is a radiological diagnosis, which clinically manifests as sudden, fluctuating or progressive hearing loss. Commonly, diagnosis is made during early childhood, either associated with inner ear anomaly, or congenital disorders; or in complete isolation. Till now, the exact pathogenesis for LVAS remains debatable.
LVAS is the most prevalent (accounting for 15 % to 20 %) cause of sudden onset of progressive hearing loss in paediatric age group (Arcand et al., 1991[1]). However this figure might still be under representative of the illness since only a fraction of patients will seek medical advice. Hearing loss is a subjective complaint. Parents might ignore their children initial complaint until later stage. Children with hearing loss may present later with delayed speech or poor academic performance.
There are two types of LVAS, sporadical and familial. The former is more common. We described 2 cases of LVAS in a Chinese family. We could not find any similarly reported familial LVAS from Asian country.
Case 1
A 14-year old Chinese girl, first of four siblings, was diagnosed with bilateral sensorineural hearing loss (SNHL) at the age of 8 years. She presented with complaint of being unable to hear her favourite television (TV) programmes clearly despite maximum volume. She denied otalgia or otorrhoea. Her developmental history was not significant. She was delivered full term, the antepartum and intrapartum were uneventful. Her parents denied any family history of hearing loss.
There were no dysmorphic features upon examination. Otoscopy showed normal tympanic membrane and on neck examination there was no goitre. Her Pure Tone Audiometry (PTA) revealed right moderate SNHL and left mild SNHL. Hearing aid was offered but the family declined.
Serial pure tone audiometry (PTA) demonstrated worsening of hearing in the right ear. There was no history of head trauma, ototoxic medications or recent upper respiratory tract infection. High resolution computed tomography (HRCT) of the temporal bone revealed bilateral enlarged vestibular aqueduct, right measures 2.8 mm and the left 2.6 mm in diameter respectively (Figure 1a and 1b(Fig. 1)).
Case 2
A 13-year old boy, second of four siblings, was noted by his parents that he was speaking louder than usual. The parents also needed to raise their voice louder in order to get his attention. Coincidently he was referred for hearing assessment since his sister (the girl in case 1) has hearing impairment. The birth history and medical history were otherwise uneventful. Another two siblings did not show any sign of hearing impairment.
His audiometry test showed right moderate to severe SNHL and left SNHL. His HRCT of the temporal bone revealed bilateral enlarged vestibular aqueduct, the right measures 2.8 mm and the left 3 mm in diameter respectively (Figure 2a and 2b(Fig. 2)).
He was fitted with bilateral hearing aid but later refused to wear them. On academic performance, he has poor grades in school as opposed to her sister; nonetheless he is still able to read and do simple mathematics.
Discussion
Vestibular aqueduct is a small J shape osseous canal in the otic capsule which follows a course from the medial wall of vestibule of the inner ear to open onto the posterior wall of petrous pyramid (Saliba et al., 2012[6]). Vestibular aqueduct continues to grow after birth and reaches adult size by the age of 3 to 4 years. Its average width of diameter in adult is between 0.4 mm and 1.0 mm (Marques et al., 2007[4]).
Vestibular aqueduct contains endolymphatic duct, a nonsensory component of the endolymph-filled, closed, membranous labyrinth. The endolymphatic duct leads from the vestibule labyrinth through the vestibular aqueduct to the endolymphatic sac. The vestibular aqueduct is visible on HRCT whilst endolymphatic duct is visualized on magnetic resonance imaging (MRI).
Valvassori and Clemis first described regarding LVAS in 1978 after analysing CT temporal of 3700 patients and concluded that vestibular aqueduct is considered enlarged when its midpoint diameter, measured from the common crus to its external aperture is more than 1.5 mm or more than 2.0 mm measured at the operculum on CT axial plane (Valvasorri and Clemis, 1978[7]).
If axial view is not available, coronal view can be used as alternative to evaluate the vestibular aqueduct and considered enlarged when midpoint diameter is larger than 2.4 mm or larger than 4.34 mm at the operculum (Saliba et al., 2012[6]). Morphology of vestibular aqueduct can be classified according to images; filiform, tubular and funnel shape. The most common morphology in adults is the filiform shape and the funnel shape in children (Marques et al., 2007[4]).
Sensorineural hearing loss (SNHL) is the most common type of hearing loss in LVAS. However, cases of LVAS with conductive hearing loss or mixed hearing loss have been documented. The presence of conductive or mixed hearing loss can lead to misdiagnosis. LVAS may present with vestibular symptoms which include vertigo and unsteadiness, where the symptoms are difficult to recognize especially in children. These impacts manifest in outward signs such as delayed reflex, visual-spatial problems, abnormal movement pattern or clumsiness.
At present, the majority of patients with LVAS received hearing aid. Cochlear implant (CI) is indicated in profound SNHL. Hearing level of patients with LVAS tends towards deterioration sooner or later. Hence in children with bilateral LVAS, an early implantation is advocated after discussing the advantages and disadvantages with parents (Asma et al., 2010[2]). An early CI application in children with LVAS will ensure them receiving the maximum amount of auditory information and a better speech recognition performance.
Whether LVAS is a hereditary or congenital disease remains as unresolved issue. LVAS typically presents solely with hearing loss. LVAS has been postulated to be inherited as an autosomal recessive trait. It may also be associated with other systemic abnormality as a part of genetic syndrome in which Pendred syndrome is the most common association. Pendred syndrome is an autosomal recessive syndrome with clinical features of goitre and severe congenital hearing loss. Other syndromes which associated with LVAS are renal tubular acidosis with deafness, Waardenburg syndrome and Brachio-oto-renal syndrome (Griffith and Wangemann, 2011[3]).
Mutation in SLC26A4 gene is closely related to LVAS in where more than 200 of SLC26A4 mutations have been described, and novel mutations are being continually identified in different countries and ethnic groups. Among Chinese patients, c.919-2A>G and p.H723R are the two most common mutations in Chinese mainland but recently Yu et al described a new 2 novel mutation; c.232T>C and c.2006A>T, of SLC26A4 gene in 6 family members of a Chinese family associated with enlarged vestibular aqueduct (Yu et al. 2010[8]).
Genetic hearing impairment may develop prelingual or postlingual. Prelingual hearing impairment has a devastating effect on language and speech development, thus an early detection of congenital hearing impairment is essential. Genetic factors have been estimated to contribute more than 50 % of permanent hearing loss in children (Parving, 2007[5]). The genetic studies will benefit in studying the correlation of disease with genetic mutation. However, the test is expensive and not cost effective. Even with the availability of genetic studies, it will not change the principal management of the diseases.
References
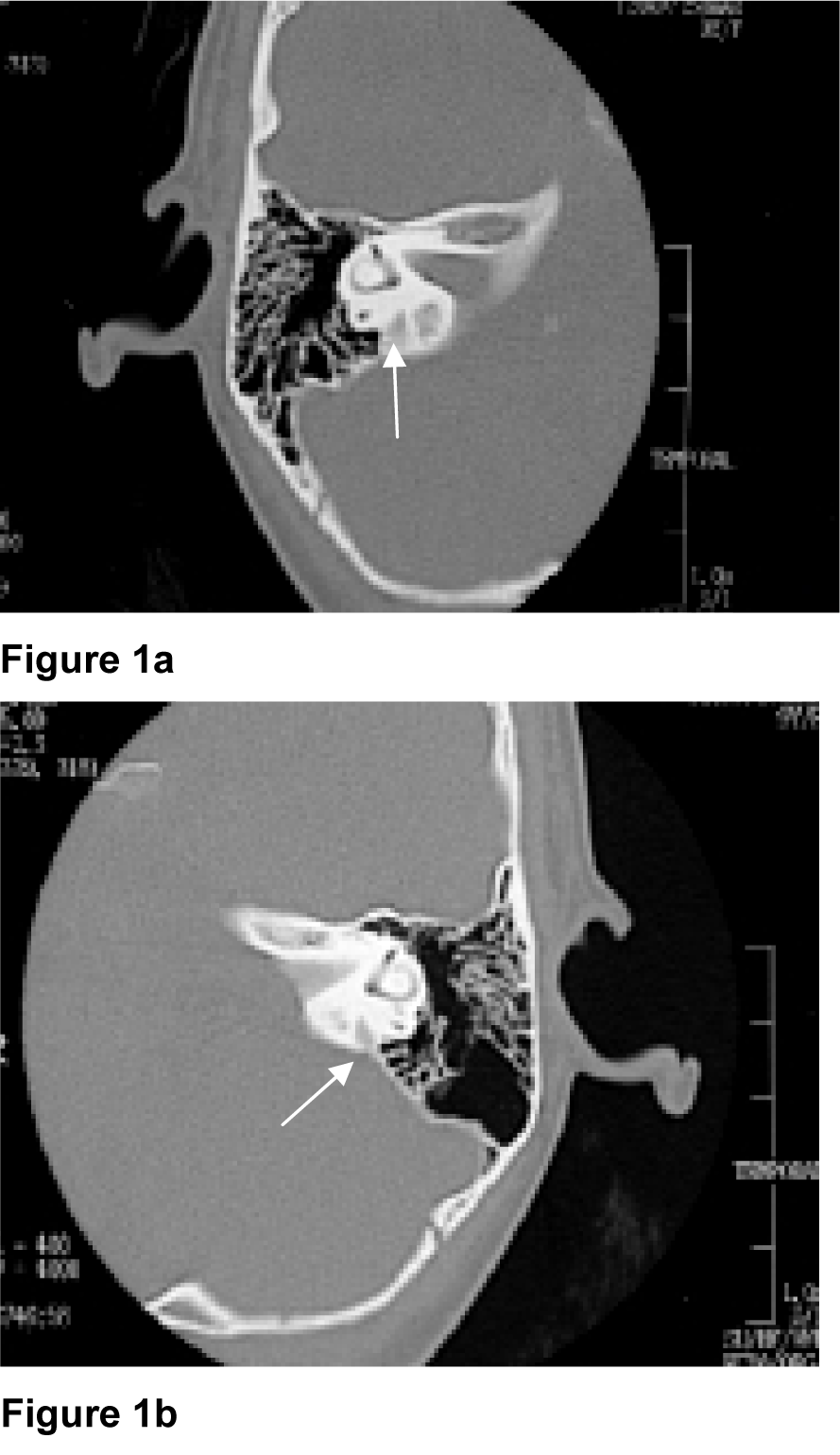
Figure 1a and 1b: Axial HRCT of the temporal bone of Patient 1, demonstrating enlarged right and left vestibular aqueduct (white arrow) respectively.
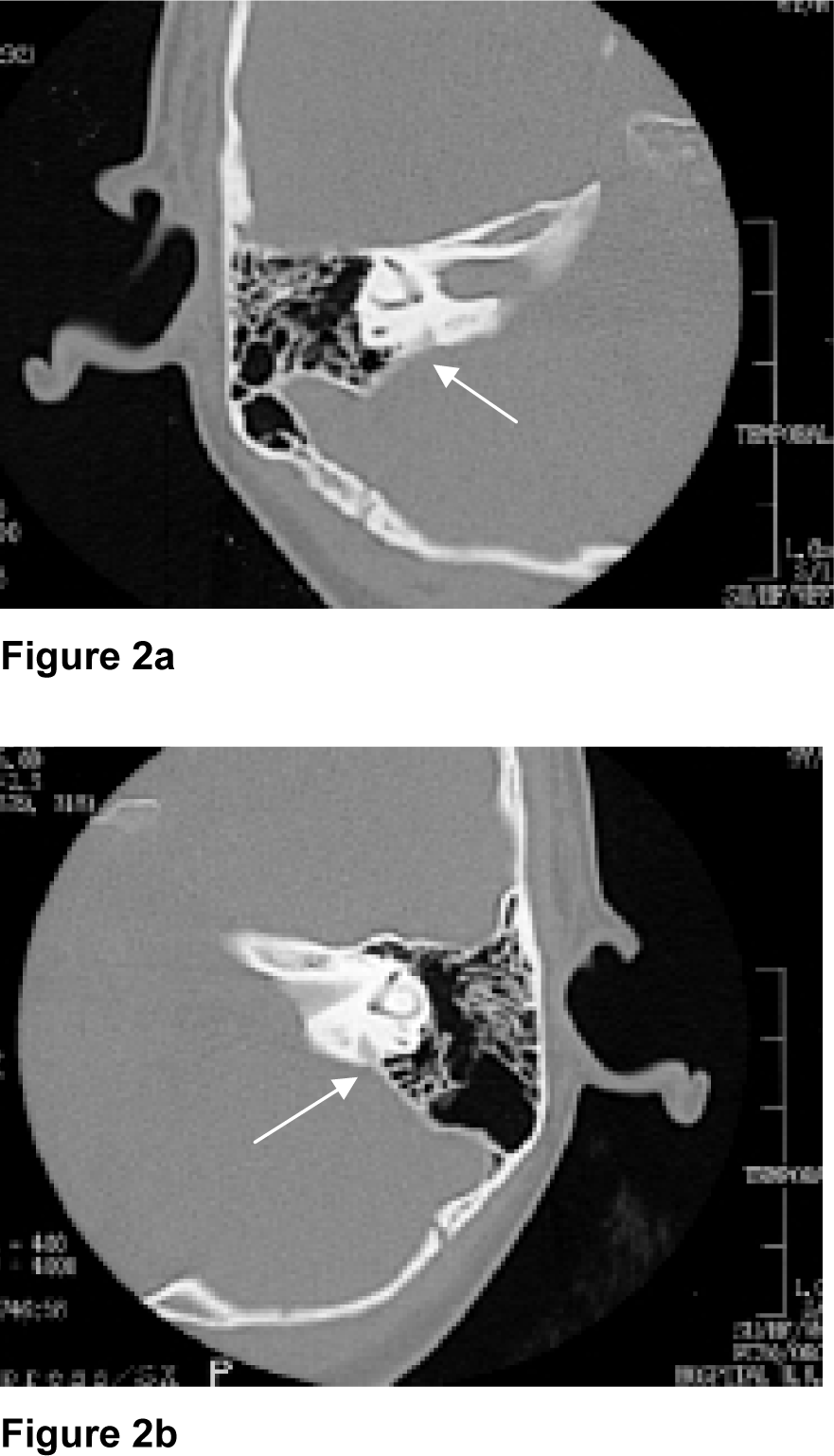
Figure 2a and 2b: Axial HRCT of the temporal bone of Patient 2, demonstrating enlarged right and left vestibular aqueduct (white arrow) respectively.
[*] Corresponding Author:
Dr. Mohd Hazmi, Department of Otorhinolaryngology, Medical Faculty, University Kebangsaan Malaysia, Jalan Yaacob Latif, 56000 Cheras, Kuala Lumpur, Malaysia. Tel: +603 91456045, Fax: +603 91456675, eMail: h_zfh@yahoo.co.uk